Abstract
Two ‘push’ factors drove Australian malariological research in the decades before World War II. The first was the
nation’s own experience of malaria in its tropical north, where local, usually seasonal, outbreaks of the disease
occurred fairly regularly. The second was the Army’s experience of malaria during overseas deployments. During the two inter-war decades, the 1920s and 30s, Australian research into tropical diseases generally and malariology in particular benefited from the return to civilian life of former Australian Army Medical Corps (AAMC) medical officers who had seen malaria at first hand during World War I. A small but significant number of them specialised in tropical medicine post-war in either the specialist medical research institutes or university medical faculties. As the war ended they began publishing their findings. This corpus of research reports was the ‘soil’ from which Australian malariology grew.
Introduction
Part 1 in this series of articles, ‘Pioneers of Australian military malariology’, profiled the careers of five AAMC officers and one civilian tropical diseases specialist who had direct experience of malaria during the first two decades of the twentieth century. In the Australian Army, malaria had been diagnosed among troops of successive contingents sent to South Africa during the Boer War of 1899–1902. The Army suffered its first two epidemics of the disease
during the next war, World War I, in New Guinea in 1914–15 and in Syria in 1918.
Part 2 in the series now examines the next two decades, the inter-war period, when tropical medicine emerged as a separate field of specialisation in Australian medical science. As in Part 1, the frame of reference is biographical. Part 2 will profile a group of former AAMC officers who either published reports on their experience of malaria during World War I or, specialising in tropical diseases, carried Australian malariology further during the 1920s and 30s.
In great contrast to World War I and later World War II, the AAMC undertook no anti-malarial work of any
kind during the two interwar decades. There were three main reasons for this:
• The AAMC had no staff for research because its commander, the Army’s Director General of Medical Services (DGMS) was the only full-time staff member.
• Except for the DGMS, all the AAMC medical officers were members of the reserve forces; and so their soldiering had to be fitted into their spare time in their busy professional lives.
• Malariology was the province of several organisations specialising in tropical medicine, most notably the Australian Institute of Tropical Medicine in Townsville and later (from 1930) the School of Public Health and Tropical Medicine at the University of Sydney.
Despite that, various Army- and war-related research papers and a book about malaria were published in
Australia between the two World Wars by veterans of the World War I campaigns against malaria. Further,
the Army’s experience of malaria during World War I helped shape Australian knowledge of the disease and consequently helped prepare the AAMC for its struggles against the disease during World War II.
The 1920s: malaria reportage in The Medical Journal of Australia
The material published on malaria during the interwar decades included most notably what appeared in the chapters by Rupert M. Downes, F. Arthur Maguire and Raphael W. (‘Ray’) Cilento in the first volume of A. Graham Butler’s official Australian medical history of World War I, The Australian Army Medical Services in the War of 1914–1918. These chapters were referred to in Part 1 of this series.
In addition to Butler’s encyclopaedic work, various papers by former AAMC medical officers were published in the Medical Journal of Australia (MJA) during the 1920s.
The first of the MJA articles was by Colonel Robert Fowler (1888–1965), who went on to a distinguished
career as a gynaecological surgeon and medical statistician.1 His article ‘The risk of malaria in Australia’ appeared in the MJA in August 1919.2 The second, ‘Incidence of malaria amongst troops on a transport to Australia from Egypt and Palestine’, was written by Colonel Walter Ernest Isaac Summons (1881–1970).3 It was published in the same MJA edition as Fowler’s article.4 Both articles alerted the medical profession in Australia to the likelihood that
troops repatriated from the Middle East would have returned home with malarial infections and could become malaria carriers in Australia.


The Commander of Anzac Division Medical Services, Colonel Rupert Downes (centre, front row) and his staff,
which comprised medical officers of both the AAMC and the Royal Army Medical Corps, Palestine, 1917. Colonel
Robert Fowler (inset) is sitting at the left. (Australian War Memorial [AWM] photograph no. H02522.)
‘In the near future,’ Fowler wrote, ‘practitioners will be called upon to treat a considerable number of malarial recurrences in men discharged from the Australian Imperial Force (AIF), many of which will be malignant, and therefore liable to be rapidly fatal.’5 By thus opining, Fowler demonstrated the limited knowledge of the era. At the time the medical profession insufficiently recognised that ‘malignant’ malaria, i.e. the falciparum form of the disease, did not recur because it has no dormant phase in the liver as does the vivax (‘benign’) form of the disease.
Fowler went on to opine that ‘unless prevented, there will be widespread infection of Australian anopheline
mosquitoes, with both benign and malignant parasites and a consequent increase [in malaria cases] in endemic areas’.6
A third MJA article was by Major Wilfred Evans MC (1889–1958). Evans had briefly served as the ‘Principal Medical Officer (PMO) of Damascus’ with the Desert Mounted Corps during the catastrophic malaria epidemic in Syria during October 1918.(The epidemic was described in Part 1 in the series.) Evans’s article, ‘Anti-malarial work with the Australian Mounted Division in Palestine, which appeared in the MJA in December 1919, summarised
the anti-malarial effort in the lower Jordan valley during the summer of 1918.7

Major Wilfred Evans MC, who served as the Principal Medical Officer of Damascus with the Desert Mounted
Corps during the malaria epidemic in Syria during October 1918. (Australian War Memorial photograph no.
H00034.)
The articles by Fowler, by Summons and by Evans were the first of a series of articles and reports trickling into the MJA from the wartime experiences of AAMC officers who had treated malaria and other tropical diseases. Among these was an item by an officer who would lead the AAMC’s anti-malarial effort during World War II — Lieutenant-Colonel (later Brigadier Sir) Neil Hamilton Fairley.8 During his service in the 14th Australian General Hospital
(AGH) at Abbassia in Egypt, Fairley had made a special study of bilharziasis (schistosomiasis), which he had reported in the Journal of the Royal Army Medical Corps in April 1919.9 The MJA duly drew attention to this achievement.
Colonel Walter E.I. Summons, who commanded the 14th AGH at Abbassia near Cairo. He treated many of the
malaria victims evacuated from Palestine and Syria during 1918. (AWM photograph no. B00661.)
Each of the four AAMC officers just mentioned had served with distinction in the Middle East during World War I. Both Fowler and Evans were in the Desert Mounted Corps. Fowler was awarded a military OBE and was mentioned in despatches three times. Evans also received three mentions in despatches as well as the Military Cross. Summons, who had served in both the Middle East and in France, ended the war as the commandant of the 14th AGH at Abbassia. He was mentioned in despatches and awarded the OBE.

Colonel (later Brigadier Sir) Neil Hamilton Fairley as the Director of Medicine, Allied Land Forces Headquarters,
Melbourne, about 1943. (Wikimedia photograph.)
Fairley, who will be profiled in detail in a later article in this series, worked at the 14th AGH at Abbassia, where he became the senior physician and made special studies of dysentery, typhus and malaria. He became interested in tropical medicine as a specialty under the influence of Lieutenant-Colonel (later Sir) Charles James Martin (1866–1955),10 with whom he worked in the Anzac Field Laboratory. In August 1916 Martin had established the Anzac Field Laboratory. (As described in Part 1 of this series, the Laboratory provided an indispensable pathological
testing service for the AIF in the Middle East during the desert campaigns of 1916–1918.) Fairley, too,
was mentioned in despatches and awarded the OBE.11 Fowler, Evans, Summons and Fairley later served again with the AAMC during World War II.
Fairley would become a truly pivotal figure in international malariology. A prolific author of papers on malaria, he would become one of the great heroes of the Australian Army’s struggle against the disease. At the end of World War I he spent two years working with his Anzac Field Laboratory mentor, Charles Martin, at the Lister Institute of Preventive Medicine in London. While there he earned a diploma in tropical health and hygiene from Cambridge
University before returning to Melbourne in 1920 to an appointment at the Walter and Eliza Hall Institute of Medical Research.12
Before returning to Australia Fairley produced a paper on the mortality from malignant (falciparum) malaria among the Allied and enemy forces in Palestine during the war. He and his co-author, a Captain H.R. Dew of the Royal Army Medical Corps (RAMC), presented their findings to a meeting in London of the Royal Society of Tropical Medicine and Hygiene (RSTMH). The RSTMH, of which Fairley would later serve a two-year term as president
(1951–53), subsequently published the paper in its quarterly journal Transactions of the Royal Society of Tropical Medicine and Hygiene. The paper, which had the title ‘The causes of death from malaria in Palestine — A study in cellular pathology’,13 was the first of 20 on various topics that Fairley would publish in Transactions between 1920 and 1952, the year he was elected as a Fellow of the Royal Society of London for Improving Natural Knowledge, commonly known as simply the Royal Society. The ‘FRS’ (Fellow of the Royal Society) postnominals are arguably the
most prestigious of all for a scientist. In Fairley’s case they would earned largely for the research he published in the Transactions.
Fairley’s and Dew’s London presentation to the RSTMH reported their findings after their postmortem examination of blood slides from 80 wartime victims of falciparum malaria in Palestine. In preparing their study they had received assistance from two AAMC officers, Lieutenant-Colonel C.B. Blackburn14 and Colonel W.E.I. Summons, each of whom is briefly discussed elsewhere in this article.15
Of the 80 malaria victims whose deaths Fairley and Dew investigated, 47 were Turkish prisoners, 22 were British and Australian soldiers and 11 were Egyptians from the Egyptian Labour Corps. Only 13 (16 per cent) of the victims had died from ‘uncomplicated’ malaria, i.e. malaria alone. The rest had died from malaria complicated by secondary
infections which were largely from the simultaneous influenza pandemic. Multiple infectious agents do interact; and falciparum malaria and influenza were shown to be a particularly lethal combination in the Egypt-Palestine region on the basis of Fairley’s and Dew’s work. Their research was confirmed by other RAMC officers who had worked in the Salonika– Macedonia (modern Greece) and Mesopotamia (modern Iraq) theatres of the war.16
In 1920 soon after returning to Melbourne, Fairley presented a second paper on the subject of the recent malaria epidemics among the troops in Palestine. It was titled ‘Observations on the clinical and applied pathology of malaria’ and was delivered to the Australasian Medical Congress in Brisbane.17 Fairley’s paper provoked a lively discussion among the members of his audience, some of whom had been wartime AAMC officers. They included Major
Eustace W. Ferguson and Lieutenant-Colonel (later Sir) Charles Bickerton Blackburn (1874–1972).18
During the early 1920s the MJA continued publishing material relating to the Army’s recent experience of malaria. Among the more prominent authors of MJA articles was Major Eustace William Ferguson (1884–1927), a pathologist and entomologist who had worked in military hospitals in England, France and Egypt before commanding the Anzac Field Laboratory between August 1918 and March 1919. Major Ferguson had accordingly led the Anzac Field Laboratory through the malaria epidemics in Amman and Damascus during September and October 1918. In a paper to the Australasian Medical Congress in 1920 he outlined the malarial diagnostic work done by the Anzac Field Laboratory and the malaria diagnostic stations during these epidemics. In the post-war years Ferguson became the principal microbiologist in the New South Wales Department of Health. His interests were broad but
he was particularly interested in dengue fever and malaria and their links with medical entomology. He published numerous research papers on Australia’s fleas, ticks, biting flies and mosquitoes before his early death from nephritis at the age of 42.19

Major Eustace W. Ferguson making a microscopical examination in the pathology department of the 3rd
AGH at Abbeville, France, June 1918. Ferguson later commanded the Anzac Field Laboratory in Palestine and
Syria. (AWM photograph no. E02603.)

Major Eustace W. Ferguson and staff of the Anzac Field Laboratory, Aleppo, Syria, 1918. Ferguson is sitting,
centre of front row. (AWM photograph no. B01025.)
Immediately after Ferguson’s presentation to the 1920 Australasian Medical Congress there came a second paper on the wartime anti-malarial work done in Palestine and Syria. This was presented by Harvey Sutton (1882–1963), who had served as an AAMC captain in the AIF in Egypt and then in the campaigns in Sinai, Palestine and Syria. He had
commanded the No. 7 Sanitary Section of the Anzac Mounted Division and then worked with Ferguson in the Anzac Field Laboratory.20 Promoted to major in 1918, Sutton served as the Deputy Assistant Director of Medical Services (DADMS) at AIF headquarters in Cairo. He was mentioned in despatches twice and awarded the OBE. After the war Sutton specialised in public health; and when the Commonwealth government and the University of Sydney established the School of Public Health and Tropical Medicine in 1930, Sutton became the school’s first director and
the foundation professor of preventive medicine. As such, he retained an interest in the diagnosis of and
prophylaxis against malaria. During World War II the Sydney School would play an important part in providing advice and training for the armed services in tropical medicine, while Sutton himself, promoted to lieutenant-colonel, became an inspector of army camps.

Professor Harvey Sutton, Director of the School of Public Health and Tropical Medicine at the University of Sydney, 1935. (National Library of Australia photograph no. nla. pic-vn4506408.)
Lieutenant-Colonel Charles Bickerton Blackburn had helped Fairley with the research for the paper he had presented to the RSTMH in London with Captain Dew. Blackburn had served with distinction during the war. He had worked with Fairley at the 14th AGH at Abbassia, was mentioned in despatches twice and awarded the OBE for his wartime service. A leading figure in Australian medical politics, he later served a term as Dean of Medicine at the University of Sydney, where he was also a long-serving Chancellor 1941–64.

Sir Charles Bickerton Blackburn, an AAMC lieutenantcolonel in both World Wars I and II. (National Library of
Australia photograph no. vn4193824-v.)
Although aged 65 when World War II began, Blackburn enlisted in the Army and subsequently saw service as a lieutenant-colonel at the 113th AGH at Concord. His son, Charles Ruthven Bickerton Blackburn (1913– ), a physician, served with the 5th AGH in the Middle East and New Guinea during World War II. A lieutenant-colonel, he later commanded the Land Headquarters Medical Research Unit in Cairns — the unit responsible for leading the Army’s campaign against malaria 1943–46.21 We will meet Blackburn Jnr. again in the latter guise in a later
article in this series.
An Australian ‘first’ — R.W. Cilento’s book Malaria
During the early 1920s Dr Raphael West Cilento (1893–1985) emerged as one of the leading figures in Australian malariology.22 Part 1 in this series profiled Cilento in detail. It pointed out how he wrote the first Australian book on malaria. This was Malaria, with special reference to Australia and its Dependencies, published by the Tropical Division of the Commonwealth Department of Health in 1924.23

An Australian ‘first’: the title page of R.W. Cilento’s 1924 book on malaria.
Before he published his Malaria, Cilento gave a preview of his approach to the disease in a presentation to the Australasian Medical Congress in 1923. This was essentially epidemiological. Thus, he observed that the malarious zone in Australia extended north from Ingham (100 kilometres north-west of Townsville), encompassing Cape York
Peninsula and then west across the ‘Top End’ of the Northern Territory, where it extended south to the Roper River (380 kilometres south-east of Darwin), and then south-west into Western Australia to the Fitzroy River mouth near Derby and beyond that to south of Broome (160 kilometres south-west of Derby).24 The vector, he said, was ‘probably Anopheles annulipes or Anopheles bancrofti’; but he believed the culprit was most likely the former because ‘it was the only common mosquito in the regions where malaria was found and in some localities, for example on the Roper River, it existed in enormous quantities and was the sole species found’.25
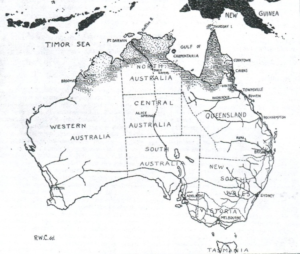
R.W. Cilento’s map of the distribution of malaria in Australia and the adjacent archipelagos. As the map
indicates, the malarious zone extends from Townsville, across Cape York Peninsula, along the Gulf of Carpentaria, across Arnhemland and through northern Western Australia to Broome. Cilento feared that the extension of the railway networks in northern Australia (marked on the map) would facilitate the rapid spread of malaria beyond the malarious zone. (Source: R.W. Cilento and A.H. Baldwin, ‘Malaria in Australia’ in The Medical Journal of Australia, 1 March 1930, p. 274.)
Cilento also expressed fears that the extension of the railway networks in northern Australia might help to spread malaria. If malaria carriers became more mobile they could carry the disease into southern regions among non-infected populations. As things turned out, the fear of malaria moving elsewhere, as dengue fever had already done from Queensland into New South Wales, was probably exaggerated. For the disease to spread further south, large congregations of malaria carriers moving into the southern regions would have been necessary, but that did not occur.
What did occur sometimes was that itinerant miners returning from New Guinea brought malaria with them, as in 1910 in the mining camp at Kidston, inland from Townsville. Infected miners from the Papuan diggings settled in Kidston in sufficient numbers to constitute a concentration of malaria carriers which then became the source of infection for the local community in an outbreak of the disease. In a population of about 400 at Kidston, 120 people
suffered malaria, of whom ‘at least 25 died’.26
Although there was no southward extension of the malaria zone, as Cilento feared, his concern was justified. The mosquito he identified as the culprit, Anopheles annulipes, has a widespread distribution in Australia, not just in the northern tropical malarious zone but in the temperate southern States as well. It occurs throughout New South Wales and Victoria and is widespread in South Australia and lowland areas of Tasmania. As a malaria vector,
this species of mosquito ‘has been responsible for the transmission of [the disease] in many areas of southern Australia’.27 It is also a vector for human filaria (the threadlike worms causing the disease filariasis), for Ross River virus (which causes epidemic polyarthritis) and for canine heartworm.28
Cilento’s Malaria received an enthusiastic review in the Medical Journal of Australia. The author, the MJA
averred, ‘is to be congratulated on the thoroughness with which he has compiled this work and on the judgement and knowledge he has displayed in handling a very large subject’.29 The book comprised four sections. The first was a general introduction to the history, causes and worldwide distribution of malaria. The second dealt with the human pathology of the disease, its symptoms, complications and treatment. The third summarised the various means
for controlling the mosquito vectors and for taking prophylactic measures to prevent malarial infection. The fourth section was an entomological summary of Australia’s mosquitoes, with an emphasis on the anopheline transmitters of malaria. ‘The usefulness of this publication and the skill displayed by the author in its compilation remain unchallenged,’ the reviewer asserted, before concluding that ‘from the point of view of the tropical hygienist the [book] deserves nothing but praise’.30
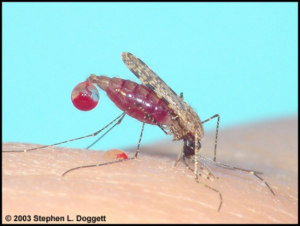
Anopheles annulipes: a malaria vector with wide-spread distribution in Australia. This particular female mosquito
has become so engorged in taking her blood meal she has begun exuding a globule of blood from her anus.
(Photograph by Stephen L. Doggett, from the website of the New South Wales Arbovirus & Vector Monitoring
Program of New South Wales Health’; reproduced with the photographer’s kind permission.)
During the year in which his book was published, 1924, Cilento returned to Rabaul as the Director of Health in the Australian administration of the Mandated Territory of New Guinea, formerly German New Guinea. He held the position for four years on secondment from the Australian Institute of Tropical Medicine (AITM). Cilento continued his study of malaria in New Guinea and published several more papers on the subject. After accepting a position
in Brisbane as the Commonwealth government’s Director of Tropical Hygiene and Chief Quarantine Officer for north-east Australia in 1928, his malariological career effectively ended.
Cilento’s last foray into malariology was a long article in the MJA in 1930 jointly written with Alec Hutcheson Baldwin (1891–1971),31 who from 1924 had been his successor at the AITM, as Acting Director. It was an authoritative paper tracing the history and the distribution of malaria in Australia. It charted the progressive decline in the incidence of the disease in Australia to the point where the annual death rate was only five deaths per million of population by 1929.32
Cilento and Baldwin attributed the decline to several factors. First, there was no large malariainfected indigenous population to form a reservoir of infection, as there was across the Torres Strait in Papua and New Guinea; and in any case, Australia’s indigenous population was diminishing. Second, Australia’s malarious zone was sparsely populated. Third, was the action of government health agencies and especially the Commonwealth Department of
Health in monitoring the occurrence of malaria and in acting quickly to manage outbreaks of the disease. Finally, and most importantly, increasingly high living standards in Australia had resulted in the populations of malarious regions being able to adopt and afford anti-malarial protective measures. In this connection they quoted the Scottish malariologist, Sir Malcolm Watson (1873–1955), who had observed that ‘the poor are malarious and the malarious
poor’.33
Cilento’s and Baldwin’s statistics could not tell the whole story of the decline in mortality from malaria in Australia because they had only the figures from 1905 to 1927. In the present era, with more than a century of figures on deaths from the disease, a more complete picture emerges. This is summarised in the following table, which relates malaria mortality to population for the century between 1905 and 2005. As the table demonstrates, the decline was both absolute and relative. From 55 malaria deaths in 1905, the number fell to just 10 a century later; and most of those ten were almost certainly individuals who had contracted the disease overseas. Expressed as a rate, ‘deaths per million of population’, the decline was from 13.75 deaths per million in 1905 to 0.49 deaths per million in 2005 — a reduction by a factor of 28 over a period when the Australian population quintupled from four to twenty million.
INSERT GRAPH
When the falling mortality rate is graphed, as below, the decline is seen to be spectacular. As mortality from malaria was falling, Australian living standards were rising, public health programs were reducing transmissible diseases to very low levels of incidence and the local pool of the malaria-infected had evaporated.
In the post-World War II decades the deaths that did occur in Australia from malaria would almost certainly have been among travellers from nearby malarious countries — Papua New Guinea, for instance — returning home to Australia after falling ill with the disease. Fewer needed to do so as the turn of the millennium approached because improved medical care in the countries Australians visited had lowered the risk of malaria for them when travelling
abroad.34

Australia’s declining mortality from malaria: the deaths from malaria in Australia over the century 1905–2005.
Cilento’s co-author in 1930, Alec Baldwin, also had a distinguished career in tropical medicine and health. He enlisted in the AAMC on graduating in medicine from the University of Melbourne in 1917 then served as a captain with the 5th Field Ambulance on the Western Front until the end of the war. After the war he remained in England, working in the Birmingham Children’s Hospital and earning a diploma in public health and later a diploma in
tropical medicine and hygiene. He then worked at Rabaul and in 1924 followed Cilento’s as the Acting Director of the AITM. When the AITM merged with the new School of Public Health and Tropical Medicine at the University of Sydney in 1930, Baldwin moved to Sydney and became the school’s Deputy Director under Professor Harvey Sutton. After World War II, as Professor Baldwin he also held the school’s chair in tropical medicine until his retirement in 1956.
During the war he had served with the RAAF as the director of hygiene and tropical health from 1943 as a group captain, a rank equivalent to that of army colonel.35
As the foregoing biographical profiles suggest, the Australian Army’s experience of malaria and other tropical diseases during World War I greatly stimulated interest in tropical medicine in Australia. Following their wartime duties with the AAMC, a small but influential group of medical officers chose to specialise in this field on quitting the AIF and several specialised in malariology. They acquired their postgraduate qualifications and experience at
universities and research institutes in England and then returned home to take up positions in the newly
established Australian medical research institutes and the universities. They presented their research findings to the meetings of the Australasian Medical Congress. The Medical Journal of Australia then reported the congress discussions and published their papers. This sequence was a major influence in keeping the medical profession in Australia informed about tropical diseases.
In relation to malaria in particular, the MJA published a continuing flow of articles, news items, editorial comment, letters and book reviews. During the two inter-war decades, the MJA ran 85 separate items on malaria. Many of these reflected on Australian advances in malariology; others reported overseas developments in the discipline. By the time World War II began, any medical practitioner who regularly read the MJA would have been reasonably well informed about the disease. Thanks to the efforts of Fairley, Cilento and their World War I AAMC colleagues who
had specialised in tropical medicine, the medical officers who subsequently enlisted in the 2nd AIF were well prepared for tackling malaria, even if not yet ready to face the epidemics of the disease that beset Australian service personnel in Papua and New Guinea in 1942 and 1943.
The 1930s: depression and a stalling of the anti-malarial effort
During the 1930s Australian research on malaria stalled. The great worldwide financial depression which began in 1929 prompted wholesale reductions in public expenditure. The resultant cut-backs in tropical medicine programs were severe. The Commonwealth Department of Health, which had been established in 1921with Dr J.H.L.Cumpston
(1880–1954)36 as its Director-General, was forced to close its Division of Tropical Hygiene in 1930. The division had been formed in 1922, had taken responsibility for the Australian Institute of Tropical Medicine (AITM) in Townsville in 1924 and had conducted enterprising research on hookworm, malaria and filariasis in northern Australia and New
Guinea. Largely as a result of the Commonwealth government’s harsh measures to reduce depressionera expenditure, the AITM was effectively closed. Its Townsville operations ceased when it was relocated
to Sydney in 1930 and merged into the new School of Public Health and Tropical Medicine of the University
of Sydney.37
The new school was jointly controlled by the university and Cumpston’s Department of Health. The AITM
name had disappeared, however; and the inclusion of the phrase ‘Public Health’ in the school’s title suggested a broader field of interests than tropical medicine alone. Those who might have hoped for a continuing sharp focus on malaria research — as at the AITM under Raphael Cilento and his predecessor, Anton Breinl — might have been disappointed that teaching would be as much a priority as research.
Perhaps Cumpston grieved privately over the demise of the AITM. Possibly, too, he opted for the pragmatic
alternative by superintending its absorption within the School of Public Health and Tropical Medicine in Sydney. His daughter Margaret Spencer, a malaria historian, later wrote that he had narrowly averted the ‘extinction’ of his whole department amidst the budgetary stringencies of the early 1930s.38 In such circumstances he possibly saw the merging of the AITM into the Sydney School as the ‘least worst’ outcome.
In forcing these changes upon Cumpston, the cost-cutting politicians and their minions in the Commonwealth Treasury might not have acted with eyes open to public health futures. If so, they could not have foreseen the malaria epidemics that broke out and claimed lives across Australia’s northern malaria zone during the mid- to late 1930s.39
During 1934 a series of widespread outbreaks of malaria in northern Australia revealed the need for concerted national effort against the disease. An epidemic of vivax malaria in the Torres Strait Islands in June that year resulted in almost a thousand (987) notifications of the disease. There were other outbreaks that year elsewhere in Queensland as well as in the Northern Territory and Western Australia. Serious outbreaks of falciparum malaria occurred in both the Victoria River and Wave Hill districts of the Northern Territory. In 1934, too, falciparum malaria was discovered in Western Australia for the first time.40
Despite the downward trend of the graph for malaria mortality seen above, the total number of deaths
from the disease in Australia between 1934 and 1939 was 96. During the next six-year period, 1940–45, there were only 60 deaths.41 Those 60, however, occurred during the wartime period of catastrophic malaria epidemics in Papua and New Guinea. During that time many of the infected troops were being repatriated to Australia for treatment, thus serving to inflate the mortality figures.
In retrospect we can appreciate that a co-ordinated approach to malaria might have prevented the outbreaks of the disease suffered during the mid- 1930s. Co-operation between the Commonwealth and the various State public health authorities in public health emergencies was a federal ideal, but the constraints of depression-era budgets precluded its realisation during the 1930s.
What the outbreaks of the 1930s might have cost the Commonwealth and States financially is probably
unknowable. We might nevertheless speculate that the aggregate public cost of all the medical investigations and examinations, hospitalisations, courses of treatment, convalescent care and invalid pensions was substantial. We might also conjecture that the cost far exceeded the expenditure that would have been required to retain the AITM in Townsville in its original form. We might even infer that timely advice from the AITM to the public health authorities
could have prevented or at least have minimised the impact of the epidemics.
Ironically, almost six decades after the closure of the AITM, an organisation that saw itself as the AITM’s successor was established in Townsville. This was the Anton Breinl Centre for Public Health and Tropical Medicine of the James Cook University. This centre was founded in 1987 in the original AITM building. It also became the base for a new professional organisation, the Australasian College of Tropical Medicine.
Administrative and institutional historians are able to take a long-term view of events like the disappearance of the AITM and the establishment of organisations fulfilling similar functions in its former premises 58 years later. They recognise that what penny-pinching politicians and bureaucrats ‘rationalise’ in one generation others must recreate
in another, often at much greater expense.
Historians also know that government agencies such as the AITM, the Commonwealth Department of Health and the Australian Army Malaria Institute are brought into being because they fulfil key functions and provide essential services in modern societies. They may be reorganised and also terminated, their functions split away and assigned to other institutions. The latter options, however, are not necessarily more cost-effective, administratively
efficient or productive of better research outcomes.
The perceived savings in financial, material and human resources may prove to be illusory.
Reverting now to the establishment of the School of Public Health and Tropical Medicine in 1930, the school started well despite the severe financial restrictions of the era. It began teaching courses in tropical medicine and hygiene and undertook mosquito survey work in New Guinea. In 1935 the school sent a medical expedition to Papua at the
request of the territory’s Australian administration. The expedition conducted malaria surveys among the Goilala, Roro and Mekeo peoples of the Port Moresby hinterland. It found that falciparum malaria was ‘hyperendemic’ among the Mekeo, with all children between two and five years of age having enlarged spleens — a reliable indicator of a community’s exposure to malaria. The expedition members experimentally used the anti-malarial drug atebrine
among the Mekeo and found it to be effective in treating malaria attacks.42
A second expedition from the school worked in Papua during 1938–39, again at the invitation of the Papuan administration. Its task was to investigate population decline among the island groups in the Milne Bay District of eastern Papua. One of the expedition members was Dr (later Sir) Edward William Spencer (‘Ted’) Ford (1902–86), who as an AAMC lieutenant-colonel would soon become a key figure in the Australian Army’s great struggle against
malaria in Papua and New Guinea during World War II.43 A later article in this series will profile Ford,
demonstrating his enormous contribution to the development of Australian malariology generally and
of military malariology in particular.
Internationally as well as in Australia the great depression of the 1930s impeded malaria research and anti-malarial programs. The Health Committee of the League of Nations, for example, had aimed to eliminate leprosy, malaria and yellow fever but the forced economies of the 1930s restricted its achievement. Politics also played its part because
the Health Committee’s Malaria Commission was compromised by its own internal divisions. The commission began by reporting on malaria control measures in the League’s member nations in 1924. Its report emphasised the point that raising living standards in malarious nations would be an important step towards eliminating the disease.
Thereafter, however, the commission was beset by internal factional disagreements over the best means for controlling malaria. On the one hand were the proponents of mosquito control; and on the other hand were the advocates of ‘quininisation’ — ridding human hosts of malarial parasites by dosing them with quinine.45
Meanwhile, the US-based Rockefeller Foundation had been promoting and funding mosquito control and
malaria eradication projects enthusiastically. During the 1930s its projects in China and Brazil enjoyed some successes.46 The League of Nations Malaria Commission was sceptical of claims the foundation made about its successes elsewhere, however. In one instance in 1927 the US Surgeon General pressured the League into withholding from publication a commission report expressing doubts about the scientific rigor of the Rockefeller-sponsored projects. This controversy revealed rivalries between the European and American malariologists. The former supported the Malaria Commission while the latter sided with the Rockefeller Foundation. Although the
USA never joined the League of Nations, this episode demonstrated that the US scientific ‘Establishment’
was powerful enough to influence the League’s health policies.47
With conflicts like these besetting malariology on the world stage, the side-show of depression-era Australian malariology remained just that. Apart from a handful of medically trained individuals at the School of Public Health and Tropical Medicine in Sydney, few Australians specialised in malariology. The best of those who did, most notably Neil Hamilton Fairley, had to seek their study and employment opportunities overseas.
This situation, however, was about to change dramatically. The malaria epidemics suffered by Australian forces fighting the Japanese in Papua and New Guinea during World War II would prompt new, intense malariological research in Australia. Part 3 in this series will show how that happened.
Abbreviations
AAMC Australian Army Medical Corps (prefixed ‘Royal’ from 1948)
AAMI Australian Army Malaria Institute
ADB The Australian Dictionary of Biography
AGH Australian General Hospital
AIF Australian Imperial Force
AITM Australian Institute of Tropical Medicine
ANMEF Australian Naval and Military Expeditionary Force
AWM Australian War Memorial DADMS Deputy Assistant Director of Medical Services
DDMS Deputy Director of Medical Services
DGMS Director General of Medical Services
DMS Director of Medical Services
FRS Fellow of the Royal Society
HQ headquarters
MJA Medical Journal of Australia
NAA National Archives of Australia
OBE Officer of the Order of the British Empire
PMO Principal Medical Officer
POW Prisoner of War
RAMC Royal Army Medical Corps
RSTMH Royal Society of Tropical Medicine
and Hygiene
USA United States of America






