ABSTRACT
The contribution physiotherapy has made to military efforts has transformed over recent decades. With the change in warfare techniques and strategy over the last one hundred years, came the development of new treatment techniques by Australian physiotherapists to deal with the multifarious and often complex injuries to Service personnel.
Advanced physiotherapy practice and modern methodologies of today have spawned treatment options for musculoskeletal injuries which enable a more rapid return to active duty than ever before in Australian military history. Additionally, physiotherapy now plays an integral role in social responsibility endeavours in the provision of civilian treatment in the local Area of Operations and in so doing advances the broader political aims linked with current military strategy.
This paper asserts that physiotherapy has evolved from a peripheral remedial activity to take a more central role in maintaining a vigorous and resilient operational force.
This paper offers the reader a contemporary exemplar in the military medical effort that is currently in Afghanistan.
INTRODUCTION
The role of physiotherapy in war has been to assist Service personnel to recover from an injury and to maintain the fighting capability of the Defence Force. Clinically there have been fundamental changes in treatment protocols over the last ninety five years as the profession has developed, and with this, the role of an Australian military physiotherapist has evolved from working in the rear echelons in General Hospitals to the present concept of treating injuries in Forward Operating Bases (FOB). This current shift in utilising Australian Physiotherapy Officers in this role enables commanders to maintain an effective force to carry the fight to the enemy.
DISCUSSION
The changing role of physiotherapy in warfare and the evolution of physiotherapy treatment protocols.
Masseurs and masseuses (predecessors of physiotherapists) serving in the Australian Army since 1915, usually worked in overseas General Hospitals in the rear echelons or on Australian Hospital Ships, and provided a range of treatments to injured soldiers so that they could either be returned to duty or classed as an invalid and sent back to Australia (Wilson,1995).
Horrific injuries to Service personnel from gunshot and artillery shells during World War One (WW1) required comprehensive treatment and rehabilitation to restore function to the effected area. The treatment provided by the Army Massage Service was far greater than rudimentary massage and was soon recognised as not only being essential to the recovery and welfare of injured Soldiers but also as an important adjunct to their overall medical care. As early as 1915, the Director General of Medical Services recognised the valuable service that the Army Massage Service provided; he advised that “joint injuries can be set at once, provided they are transported on ships with facilities for massage, simple electrical treatments… As regarding nerve injuries following necessary surgery, as soon as the wound is healed facilities must be provided for their continued treatment on the ship by splinting, massage, electricity” (Wilson,1995). Other treatments of the day consisted of massage and hot air baths to open wounds, which had been treated with zinc or copper ionization. An illustration of the amount of work that the Army Massage Service performed is summarised by Butler (1943) who stated that on any given voyage, three thousand treatments were provided to convalescing troops on their return to Australia. Of the different types of injuries seen, Staff Sergeant Beck, a masseuse, wrote in 1916 from Mena House Hospital in Egypt, that “there were plentiful supplies of injuries to knees, ankles, and lumbago” (Wilson, 1995).
Much like the advancement of medicine through war, a wider concept of physical therapy emerged towards the end of WW1; that being the recognition and incorporation of remedial exercise aimed at the attainment of a functional result. From this concept, the term ‘physiotherapy’ and its philosophy in the restoration of movement and function through manual treatment and exercise therapy, emerged.
At the commencement of World War Two (WW2), physiotherapists were again called upon and were eventually incorporated into the Australian Army Medical Corps. During this period, several different and new treatment approaches were developed to assist in a soldier’s recovery and to restore function. Innovative treatments were developed in line with injuries, such as graduated limb movements in heated saline baths for severe burns, massaging skin grafts with lanoline, treatment of hand injuries and the extended use of remedial exercise therapy. The concept of assisting and instructing in human movement came into being from the physiotherapist’s use of passive and active movements to mobilise stiff joints following closed procedures for wounds in plaster casts. When procedures changed to open wound management, the physiotherapist vitalised the skin graft by friction massage movements using lanoline. Much like their WW1 predecessors, physiotherapists continued to remain in the rear echelons, providing secondary care with the view to restoring a serviceman’s physical capabilities, enabling them to return to full duty or repatriation back to Australia.
It was not until the Vietnam War that the need for a physiotherapist well forward in the battle space was recognised. Three physiotherapists were deployed in succession with the 1st Australian Field Hospital in Vang Tau from 1969 to 1970 and undertook chest care in the Intensive Care Unit to soldiers following injuries caused by mine explosions as well as in short term rehabilitation to those who were injured by minor gunshot or fragment wounds (Liebich, 2008).
Unlike their predecessors, these physiotherapists worked close to the fighting, and now this role has evolved further in the modern military Physiotherapist’s expanded role in conflicts such as East Timor and Afghanistan.
In today’s theatre of operations, such as Afghanistan, unconventional warfare has taken on a more dominant role compared to previous conflicts. The need for Forward Operating Bases to combat this type of warfare has necessitated the requirement of fully supported units, and with this, the deployment of Australian Physiotherapy Officers within the Area of Operation (AO); whose role is similar to that of previous conflicts but with one important difference – a greater emphasis on restoring the physical impairment of an injured soldier and returning them back to their unit in the shortest possible time, thereby maintaining the fighting capability of the force.
This major difference between the historical role of physiotherapy in previous conflicts and the present role of maintaining a unit as an effective fighting force at the coalface is fundamental. Not only is it costly to repatriate a soldier back to Australia for physiotherapy but there is also the issue of a unit’s fighting capability being eroded from the loss of key personnel – two important factors that require remediation. A deployed Physiotherapy Officer with the unit’s medical asset has several very important advantages; it compliments the delivery of primary health care by resolving musculoskeletal pain and dysfunction; is a valuable resource to the Commander by providing an injury recovery timeline for injured personnel and injury prevention strategies; and is a force multiplier, achieved by maintaining the fighting force by facilitating the recovery of acutely injured soldiers using manual therapy and specific exercise programmes thus providing the ability to return them back to their unit in the shortest possible time in the AO.
As a Physiotherapy Officer who was deployed to Tarin Kowt, Afghanistan, in 2009-10, the author had first hand experience in this paradigm shift in the role of an Australian physiotherapist on active service. Deployed with the Regimental Aid Post (RAP) for six months, the author assessed and treated many musculoskeletal injuries that would have either resulted in a serious impediment to the soldier’s performance whilst on a mission or to be evacuated back to Australia for rehabilitation. Not only were the unit’s ‘operators’ (front line fighters) treated but also personnel from Combat Service Support (cooks, drivers, mechanics, electricians, stores and medical personnel) who have the important function of sustaining their capability. Having a Physiotherapy Officer on base ensured that all personnel of the task force could access immediate treatment, thereby sustaining the Force’s combat capability.
Although the types of injuries assessed were much like those that Staff Sergeant Beck experienced back in 1916, the important difference in 2010 is that recovery time would be quicker as treatment was commenced immediately, and continuity of active service was maintained for the soldier while being treated on location. This last point is of great importance as the ‘operator’ is able to keep current in regards to training and missions whilst being treated, thereby maintaining the operational tempo. Furthermore, it was also found that the demand upon the medics and Medical Officer was also reduced in terms of treating musculoskeletal injuries by the presence of a Physiotherapy Officer, thereby freeing their time for other types of ailments and tasks.
Common injuries and key treatments in Afghanistan.
The majority of musculoskeletal injuries assessed in Afghanistan were usually caused by load carriage whilst patrolling beyond the FOB or from gym exercises on base. The types of injuries were many and varied, including facet joint dysfunctions of the spine and ribs, Lumbar disc strain, radicular and somatic pain, rotator cuff strains, knee & ankle sprains and tendonitis. These can be quite debilitating to the individual – affecting the ability to run, twist, turn, carry loads, and reducing the response time to drop to the ground if under fire. This reduction in the soldier’s optimum performance under combat conditions poses not only a risk to that individual, but also a significant loss to the effectiveness of that section and to the fighting capability of the unit as whole. Other types of injuries, such as burns, blast and gunshot wounds were rarely seen by the author as they were usually sent back to the Role 3 Hospital in Kandahar or Germany and then later transported back to Australia for further treatment depending upon severity.
The skill sets of today’s physiotherapists have built upon those of WW1 and WW2, having similarities in the basic therapeutic approach but with some major differences which lend themselves well to the current employment of physiotherapists in a FOB. Apart from the use of manual therapy, which is “a broad group of skilled hand movements used by the physical therapist to mobilise soft tissue and joints for the purpose of modulating pain, increasing range of motion, reducing or eliminating soft tissue inflammation, inducing relaxation, improving contractile and non-contractile tissue extensibility and improving pulmonary function” (Bottomley, 2000), the development of manipulative therapy (the application of accurately determined and specifically directed manual forces to the body to improve mobility in areas that are restricted within joints, in connective tissues or skeletal muscles. Korr, 1978) over the last four decades has continued this trend in providing the delivery of effective treatment outcomes to patients that have been observed clinically. These skill sets provide the Physiotherapy Officer with a much broader range of treatment options than their predecessors, enabling them to deliver a more effective and responsive treatment regime.
The author found that management of a musculoskeletal injury at Tarin Kowt often involved a multidirectional treatment approach to obtain the desired outcome. This could consist of a combination of manipulation (a high velocity but short thrust of the effected joint of the spine) or mobilisation (graded oscillations to a peripheral or spinal joint), correction of muscle length and strength imbalances, dry needling, neural mobilisation, and individually graded exercises that took into account the type and degree of injury and the operational time constraints of the individual. It is this type of treatment approach that enabled soldiers to be rapidly rehabilitated on site and represents a significant shift in the role of an Australian military physiotherapist.
Physiotherapy statistics from the previous three years at Tarin Kowt demonstrated that musculoskeletal injury to the spine had the highest incidence above all other types of injuries. Two examples the author encountered in Afghanistan were Lumbar disc strain and facet joint dysfunction of the spine. Lumbar disc strain and disc derangement, usually caused by load carriage (carrying weighted back pack, body armour and helmet, weapons and ammunition), or long periods of sitting while being driven over rough terrain, resulted in a reduction to the individual’s trunk range of movement and difficulty to transfer between standing, sitting or lying due to pain. This injury can severely debilitate the soldier for many weeks and even risk being returned to Australia for treatment. Physiotherapy treatment was very successful in resolving this type of injury by using strapping tape to off load the disc (picture 1), mobilisation to the lumbar spine to restore segmental movement to the area, McKenzie Lumbar extension exercises to facilitate this movement and core strengthening exercises to maintain the correction.
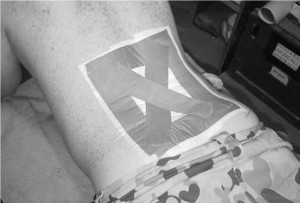
Picture 1. Taping the lumbar spine to off load the disc.
Facet joint dysfunction, which was mainly caused by load carriage, or possibly due to constriction on spinal joints whilst wearing body armour or a combination of both, was also a common injury and often involved the lumbar, thoracic or costovertebral facet joints. This injury can severely restrict movement due to localised pain and associated muscle spasm and greatly hinder the soldier in the field. Movement and function was usually restored very quickly by a localised manipulation (picture 2) to the facet joint with the soldier promptly returning to combat duties, often within 24 hours.
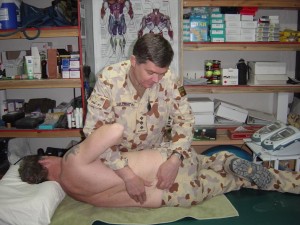
Picture 2. Performing a localised lumbar manipulation.
Another key treatment tool used to facilitate segmental mobility and restore function to a facet joint is mobilisations (picture 3). This treatment can also reduce radicular pain by altering the patency of the spinal foramina and affecting the corresponding exiting nerves. The soldier in picture 3 was experiencing radicular pain extending from the lower cervical spine and down both arms. His condition was successfully managed with mobilisations and he could remain in the AO as an effective member of his combat unit.
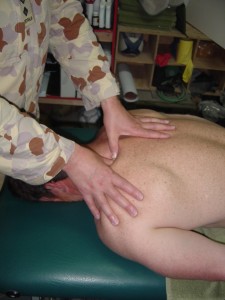
Picture 3. Mobilisation to the lower cervical spine.
The role in Counter Insurgency (COIN) and Stability Operations.
Another major difference in the role of physiotherapy in Afghanistan compared to previous conflicts was assisting with the medical care of local Afghans. Counter Insurgency (COIN) and Stability Operations are now a large part of military strategy designed to capture the “hearts and minds” of the local populace as a means of securing a long term and stable resolution. In keeping pace with this philosophy, physiotherapy can play a major part, which contrasts to the physiotherapy role of yesteryear. The author was fortunate to have the opportunity to assist the American Forward Surgical Team (FST) at Tarin Kowt to treat local Afghan civilians, who had suffered from various injuries, often orthopaedic, through accident or conflict (pictures 4 & 5). The use of manual therapy and exercise prescription was administered to facilitate their recovery and the provision of this health service to local Afghan people ennobled the Coalition Forces in their minds thereby contributing to this important COIN concept.
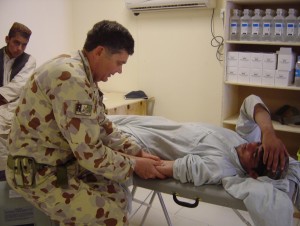
Picture 4. Joint mobilisation of the elbow to improve movement.
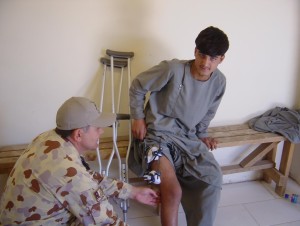
Picture 5. Instructing exercises for the knee.
Future developments in treatment protocols
Future treatment protocols for physiotherapists in the Australian Defence Force (ADF) could parallel that of developments currently being undertaken in the Australian public hospital sector. Physiotherapists are now employed in Emergency Departments of many major hospitals, providing assessment, treatment, and advice to patients with acute orthopaedic trauma. Australian military physiotherapists could likewise be a valuable asset in the acute trauma setting whilst on deployment, giving many benefits such as non-surgical interventions, faster flow through of patients and improved patient clinical outcomes. Furthermore, many public hospital physiotherapists in the UK are training as extended scope practitioners, treating such conditions as subacromial bursitis with a cortisone injection and follow up shoulder exercises. Although Australia has been slow to take up this progression, these extended skills would give the Australian Physiotherapy Officer a broader range of treatment options in the acute care setting whilst on deployment, or, in Australia treating Garrison Troops. As new skills and treatments continue to develop in physiotherapy, the need to keep pace is very important and should be reflected in the professional development for military physiotherapists. This is paramount for Physiotherapy Officers in order to continue to provide a valued and essential physiotherapy service to the ADF.
CONCLUSION
Physiotherapy as a profession has evolved through the development of new treatment techniques and methods in response to war injuries since 1915. Correspondingly, the role of physiotherapy has also changed from a small contingent of the Army Massage Service providing secondary care in rear echelon hospitals during WW1, to the present day treatment of soldiers in the primary care role well forward in the AO. Today, the ability for Australian Physiotherapy Officers to treat a wide range of conditions on site in the AO enables Commanders to maintain continuity and cohesiveness to their force to maximise operational readiness. Physiotherapy has had a long association with the Australian military service and continues to meet the challenges brought by war, making a significant contribution to the ADF.






