Reprinted with permission of the Naval War College Review
Captain Smith, a frequent contributor to the Naval War College Review, is adjunct professor in both the Department of Surgery and the Department of Military and Emergency Medicine at the Uniformed Services University of the Health Sciences in Bethesda, Maryland. He is also professor of surgery (urology) at the Medical College of Georgia, in Augusta.
The futuristic concept of joint, geographically dispersed, expeditionary (or “distributed”) operations emanating from bases at sea entails many challenges. Among them are the formulation and design of afloat casualty-care capabilities, especially where maneuver forces are inserted into territories devoid of land-based logistic support. In expeditionary amphibious operations during the past century, ad hoc creative shipboard adaptations for treatment and salvage of the combat wounded occasionally proved successful and functionally effective. If flexible and adaptive joint operational medical support is to be made available in the future, an appreciation of these historical achievements is essential. Further, if the frequently irretrievable physical deterioration of the injured—metaphorically, the “triangle of death”—is to be avoided, familiarity with the immediate needs of the combat wounded is likewise imperative, especially the unique requirements of wounds seen in contemporary armed conflict.
The Operational Context: Distributed Sea-Based Operations
Sea-based forces in the future will be involved in a wide array of missions, ranging in scale from disaster relief and humanitarian operations to full-fledged sustained combat at sea and ashore; in some conflicts, the bulk of fighting will be undertaken by joint or combined task forces. In this setting, an inclusive concept of joint sea basing—a “distributed warfighting architecture,” attuned to the strategic environment and the likely security challenges of the twenty-first century—has been proposed. A distributed network implies a transformation of maritime forces—fewer maritime platforms, geographically dispersed and integrated with organic and distributed sensor and communications nodes. It connects all the platforms and major systems deployed by the U.S. sea services—ships, submarines, aircraft, unmanned vehicles, and Marine units, as well as joint and combined forces—in a way that facilitates information sharing and affords operational commanders fully networked battle forces.
It is generally postulated that the distributed, sea-based, and networked force will be capable of countering anti-access and irregular-warfare challenges in the littorals and will be less inherently vulnerable. Consequently, it will require less force protection, and will be at less risk of catastrophic mission degradation than traditionally organized forces.1 Nevertheless, it cannot be ignored that the availability to potential adversaries worldwide of inexpensive, advanced weapons and sensors has increased the risks always associated with ship-to-shore movement. Ample respect must be given to the 250-nautical-mile range of contemporary antiship cruise missiles, as well as to the shallow- and deep-water capabilities of mines (some now incorporating state-of-the-art sensors and processors to complicate countermeasures). Furthermore, these sensors and weapons—which utilize precision, speed, stealth, maneuverability, background clutter, and surprise—will presumably target the afloat sustainment base, whose big, slow ships include prepositioned units with hulls not built to combat standards, these generally characterized as “access sensitive vessels.”2
Such ships invariably have little time to defend themselves against weapons employed at the short ranges likely in the littoral. This was exemplified by the sinking of the unarmed but strategically important British transport MV Atlantic Conveyor by an errant Argentine Exocet missile while it carried multiple helicopters to support United Kingdom forces in the Falkland Islands.3 In addition, the complicated task of preventing or rapidly detecting the laying of mines, and the subsequent difficulty or impossibility of clearing them in waters covered by a coastal defense system (including diesel submarines and missile-equipped fast patrol boats) will ultimately oblige task force ships with their medical facilities to move to seaward. That, in turn, will have major implications for casualty survival.
Avoiding The Triangle Of Death
The expeditionary logistical calculus must always include the possibility of human casualties (sickness or wounds, incurred ashore or at sea), and that reality must be factored into every operational equation. Contingency health care considerations must be integrated into plans; neglect of these critical elements can ruin any grand operational design. Unfortunately, forward medical support in an over-the-horizon insertion of forces into hostile terrain, far from supporting facilities and with no initial lodgment ashore, can be hampered by isolation and dispersal of units, obstacles to tactical radio communication, and limits on vehicular transportation. Small units will be required to extract and evacuate their own casualties, with resultant delays in meaningful treatment.
Concurrently, as a result of the current mandate for compactness and simplicity of maneuver units, landing force medical units have been lightened and downsized. Though combat operations could penetrate some two hundred miles inland, the technical capabilities of their medical assets have been lessened. All this implies greater dependence upon afloat resources, with the hopeful, but perhaps unrealistic, expectation that the sick and wounded can be rapidly evacuated to them. Unfortunately, sea-based operations may be subject to geographic limitations, making the time and distance constraints upon timely delivery of casualty care formidable. Although bases established at sea may have access to the approximately 70 percent of the earth’s surface that is ocean, ground forces employed or sustained by them only have access to land areas within range of their ship-to-shore aircraft. While various sea-basing scenarios have been structured to support operations with flight distances ranging from 110 to 220 nautical miles from the launching ships, actual inland reach for sea-based aircraft might be considerably shorter for a number of reasons: the ships in a sea base would be expected to remain “over the horizon” at least twenty-five nautical miles offshore to make them more difficult to detect and attack; sea-based ships cannot always be positioned perpendicularly offshore (for the shortest distance) from supported ground units; once over land, aircraft are likely to fly evasive flight paths to make it more difficult for an adversary to position defenses along their routes.
If efforts must be made to avoid air defenses, increases of roughly 30 percent in flight distances can be expected as well. Those considerations could reduce the effective operational reach inland to as little as sixty nautical miles for current aircraft, and about 130 for the planned longer-range heavy-lift rotorcraft. Furthermore, high terrain in the vicinity of the coast could further limit operations because the performance of rotorcraft decreases with increasing altitude. (Many parts of Iran, for example, are mountainous. Nearly 40 percent of Iran’s land area and almost half its population are located at elevations greater than five thousand feet above sea level—and would thus present limitations to flight operations, and consequently to casualty retrieval.)4
Clearly, retrograde evacuation to ships located far over the horizon may be a delicate and precarious undertaking, not only in its execution but in its impact upon casualty survival as well. The future littoral tactical environment, one of unparalleled complexity, may impede timely evacuation and medical management of casualties; an adversary may logically recognize sustainment as the force’s Achilles’ heel. Lengthy over-water evacuation may be easily thrown into confusion by sea and weather conditions as well.5
The sick and wounded are perishable cargo; whether they survive or die is fundamentally affected by the speed with which they are given medical care. The timeliness of both initial treatment and the evacuation of casualties is extremely important. Even those with potentially salvageable wounds may die or, if they survive, may experience serious complicated disabilities if treatment is not correctly timed. Early first aid, prompt resuscitation of vital functions, and initial stabilizing surgery are particularly important in this process. In essence, delay in treatment due to evacuation lag is tantamount to denial of care to those who could have survived, some without disability with early surgery.6 In addition, delayed application of treatment to initially simple wounds can facilitate their conversion into complex, infected,and often life-threatening problems.
For all these reasons, delay in surgical intervention places the wounded in what military trauma circles characterize as the “triangle of death,” where they become trapped by the triphasic onset of diminished body temperature (hypothermia), the accumulation of body products of metabolism (acidosis), and the potential for accelerated bleeding (coagulopathy).
An equally important issue is the possibility that large numbers of casualties will accumulate within the sea-based echelon, perhaps very rapidly. During the Falklands campaign in 1982, forty-six deaths and 150 surviving wounded casualties were created instantly by the bombing of the amphibious ship HMS Galahad by the Argentine air force. Most of the casualties were severe burn cases; fire has always been a prominent phenomenon following ordnance explosion within ships at sea.7 These occurrences bespeak the danger on both sides of a conflicted coastline.
Consequently, analysis must envision how casualties are generated in littoral warfare, in a continuum of operational realities both on the ground and at sea. Military planners unfamiliar with those realities often suggest that medical evacuation is but an exercise in logistics, in which the number of anticipated casualties, the capacity of transport, the time availability of shuttles, and number of beds available are the primary considerations. This view, which in effect ignores the unique time and resource requirements of wound care, accepts an overall increase in deaths, or at least disability, and the return of fewer personnel to duty. Any new concepts of casualty care must be modulated by the fact that the disturbed, tenuous physiology of the combat wounded cannot be dealt with by standard logistic formulas that equate the movement of stretcher-borne patients with that of ration boxes.8
Medical Care at Sea
The history of successful expeditionary medical support demonstrates above all the importance of adaptability and creativity in afloat casualty care. However, the beginnings of sea-based medical support were not auspicious.
Starting from Base Zero: Nelson’s Blood
During the eighteenth century, medical care aboard warships was universally poor.9 The British navy, because of its low social status, poor living conditions, and long stays at sea, attracted only the lowest-quality surgeons, mates, and physicians. On most vessels, surgery and medical treatment were performed in “the cockpit,” a small, low, crowded, poorly ventilated, dimly lit room, far below deck. Surgery often involved amputation. The patient was given rum, some other liquor, or opium, if available, and a piece of leather to chew on while the cutting was accomplished. The mortality rate was profoundly high.
But there was no system for evacuating the wounded from battle stations to surgery in the first place. Sailors dragged themselves to the cockpit or were helped by comrades (for which they could be flogged for deserting their stations). Neither was there any system of triage. The wounded presented in line for medical attention; the small complement of medical personnel enforced no priority. Thus, a slightly wounded sailor might be treated while more severely wounded succumbed to shock and bleeding. It was customary to leave patients to recover in hammocks in small areas separated, sometimes, by canvas partitions; these primitive sick bays were located out of the way, in the darkest, least used, and worst ventilated spaces of the ship.
When ground forces were transported, overcrowding increased and losses to disease aboard ships were often higher than normal. To deal with the problem, the Royal Navy provided “hospital ships” to carry the sick, but these vessels generally had no medical personnel aboard, and other ships’ physicians were forbidden to leave their own vessels to help. These “hospital ships” became little more than stinking, disease-ridden, floating warehouses where the ill were kept until they either recovered or died.
The French and Spanish navies attempted to return their dead to home port, but in the British navy they went overboard; in fact, a wounded British sailor unable to make his way to surgery was likely to be thrown overboard while still alive. A physician accompanying Lord Cathcart’s campaign in the West Indies in 1739 described the conditions on board: “The men were pent up between the decks in small vessels where they had not room to sit upright; they wallowed in filth; myriads of maggots were hatched in the putrefaction of their sores, which had no other dressings than that of being washed in their own allowance of brandy.” The ships described were anchored in the harbor of Cartagena (in present-day Colombia); the dead were thrown overboard, where they floated while sharks and birds of prey fed on them in full view of the surviving patients. The latter practice was operative when the legendary Vice Admiral Horatio Nelson, commanding the British fleet at the battle of Trafalgar in 1805, was struck by a bullet that entered his shoulder, pierced his lung, and came to rest at the base of his spine. He retained consciousness for four hours, during which he reportedly begged the flagship’s captain, Thomas Masterman Hardy, not to have him thrown overboard. Captain Hardy agreed, and when Nelson succumbed to his wounds his body was sealed in a cask of brandy for transport back to his father’s parsonage.10
World War II: The LST(H) and the 7th Amphibious Force
Clearly, medical care at sea has evolved since the eighteenth and early nineteenth centuries. Vice Admiral Daniel Barbey, commander of the 7th Amphibious Force in the Pacific theater during World War II, later noted of his ship’s innovative medical capabilities:
Even before battle casualties started coming in, the staffs of the amphibious ships in Milne Bay [New Guinea] were unequal to the task of caring for those stricken with tropical diseases. There was doubt that a hospital ship would be assigned to the Seventh Amphibious Force… but as a partial substitute we thought we might be able to convert an LST [tank landing ship] into a “first aid” ship if we could spare one and if the Navy Department had no objections… Anyhow, an official request was sent to Washington outlining our reasons and needs. Then, to “save time” we went ahead with the LST conversion plan on the assumption that it would be approved… The LST 464 was chosen because she would arrive in Sydney within a few days where the shipyards could do the work. Two days after her arrival the conversion job was under way and her character changed from a fighting ship to a ship of mercy… Assembling equipment in the States would not have been a matter of consequence, but getting it in war short Australia required a lot of priorities. The ship’s medical staff… were obtained by “thinning out” other ships and shore bases.11
LST 464 subsequently became the main reliance for medical service in the 7th Amphibious Force. In early operations it was stationed at advanced bases to receive casualties from other amphibious craft for transport to Milne Bay. As other ships joined the force and operations became larger, additional units were converted into “casualty ships.” Surgical teams were embarked for the emergency handling of 2016the wounded evacuated to these medically outfitted ships, designated as LST(H)s. These special LSTs, which like normal units carried combat troops and equipment to the assault, could remain “beached” for surgery after disembarking them. Planners saw the value of using LST(H)s this way in the Philippine Archipelago in 1944 at the battle of Leyte Gulf, and also of holding one or two in reserve, to be committed to beaches overwhelmed with casualties or without medical facilities. As recalled by Admiral Barbey, “Since Army hospitals ashore could not be set up as rapidly as anticipated because of heavy rains, LST 464 remained in the harbor and became the most important medical facility afloat or ashore for several days.”12
Admiral Barbey concluded, “Our first aid ship did a magnificent job throughout the war. Ironically, nine months after her conversion, and after she had handled some thousands of sick and wounded, a letter was received from the Bureau of Ships regretfully turning down our conversion request: ‘It is desired that all LSTs continue to operate in the manner for which they were designed.’ The letter was placed in those files most likely to be lost in combat, and the LST 464 continued to operate, if not in the manner for which designed, at least in the way we most needed her.”13
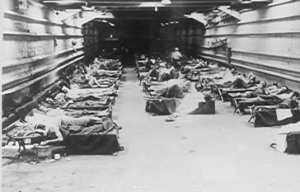
Casualties being brought aboard a beached LST (U.S. Navy Bureau of Medicine and Surgery Historian)
An LST tank deck with casualties (U.S. Navy Bureau of Medicine and Surgery Archives, BUAER 435557)
The Evolution of Hospital Ships
During the operation at Lingayen Gulf in 1945, six LST(H)s were beached to provide surgical care. At Normandy in 1944, all LSTs were equipped to handle returning casualties, and fifty-four were outfitted to perform surgery. Others were subsequently equipped to serve as casualty control ships, regulating the retrograde flow of the wounded to rear facilities. One was even made into a floating blood bank. Such hospital LSTs, able to provide surgical care in a relatively safe environment close to shore, performed even under fire at Iwo Jima and Okinawa.
World War II
Another scenario-driven innovation of World War II that contributed to the evolution of modern hospital ships was a group of three APHs, converted personnel transports with medical modifications. The attack personnel transport (APA), although not designed or equipped to handle casualties, often bore the brunt of initial casualty transfers from beach assaults—for example, at Iwo Jima. An APH (which could carry landing forces inbound) was considered preferable, because it had a complete staff of medical specialists and a large sick bay, so specialized treatment could be administered. Operating outside Geneva Convention protections, the camouflaged and heavily armed APH carried eight to twelve medical officers and sixty hospital corpsmen (no nurses were assigned). Each ship was capable of transporting 1,150 patients, with three hundred beds reserved for major casualties, two main operating rooms, and two auxiliary surgical facilities. These ships, built upon freighter hulls and equipped with Higgins-type LCVP landing craft for shuttling casualties from shore, were held in the “transportation area” of the assault force as evacuation ships. When bed capacity was reached, the ships sailed, to avoid further exposure to air attacks. As a general rule, APHs withdrew out to sea at night, but on occasion they remained anchored about a thousand yards offshore, protected by smoke screens.
Upon U.S. entry into World War II, the Army Transport Services generally assumed responsibility for evacuating Army sick and wounded, carrying them in the hospitals of troop transports. During the amphibious campaigns in the Mediterranean, small craft returning with casualties to transports or hospital ships transferred their patients by litter hoist or by hoisting the ambulance boats themselves to the rail and then transferring the patients directly to the deck. The most expeditious method was to keep one boat, usually a disabled one, permanently rigged for hoisting; ambulance boats would come alongside and directly transfer their casualties to it.14
The troopships offered neither comfort nor sufficient care, and there was no guarantee against enemy attack. Consequently, admirals William F. Halsey and Chester Nimitz decided instead to use Geneva Convention–protected ships whenever possible, to evacuate those who needed considerable medical care en route and would be unable to abandon ship without assistance in an emergency. By early 1944, the Comfort (AH 6), Hope (AH 7), and Mercy (AH 8) had been converted and placed into service with civilian crews and Army medical staffs. Ultimately the Army had twenty-six such ships, the majority converted passenger liners or troopships. Two Navy hospital ships had been in commission in 1941; three were added in 1944 and seven more in 1945. During the final phases of the Pacific campaign, tactical doctrine for employment of Navy hospital vessels changed, allowing them to function as mobile, definitive-care combat hospitals rather than as transports only. Specially designed ships of the Haven (AH 12) class were also built to support this concept, which was to continue through the recent conversion of tanker hulls to produce the current Mercy (T-AH 19) and Comfort (T-AH 20). At Leyte Gulf, however, it became apparent that floating hospitals were urgently needed at the objective, especially during the night, when hospital ships were under orders to retire. Two arriving APAs were summarily designated as casualty receiving ships and stationed offshore to provide hospitalization at night. Small escort patrol craft, PCE(R)s, were also used as ad hoc transports for casualty evacuation.15
(Official U.S. Navy photograph)
The Korean War
During U.S. Marine landings at Inchon, LST(H)s once again demonstrated their value in immediate medical support of combat operations. Concurrently, two United Nations hospital ships supplemented by five U.S. hospital vessels served as seaborne ambulances, and later as definitive-care platforms. Their original mission was to transport casualties to Japan, providing care en route, but Korean conditions made them far more valuable as rear-area hospitals. Some shuttled between Korean ports as mobile hospitals; others remained in port for considerable periods conducting clinics similar to those of land-based facilities. Patients were winched aboard from docks or from lighters and landed in helicopters. USS Haven (AH 12), however, arrived in Inchon Harbor without a flight deck; its innovative commanding officer improvised a deck with pontoon sections obtained from the Army, mooring them perpendicular to the anchored ship on both sides and equipping them with warning lights, wind-direction indicators, and firefighting equipment. Rope ladders and temporary gangways provided access. Up to four helicopters could be landed and their casualties brought aboard ship with litter hoists.16
USS Haven at Inchon, 1952 (official USN photograph 445542, August 1952)
The Falklands
In 1982, in anticipation of the campaign to retake the Falkland Islands, Britain’s Royal Navy requisitioned two commercial cruise ships, SS Uganda and SS Canberra, and refitted them for casualty care. The P&O ship Uganda, already containing hotel, laundry, and other facilities required for patient care, was converted and painted white, with red crosses, in Gibraltar within sixty hours. A helicopter pad was fitted, as well as a ramp for rapid transfer of patients to the main hospital on the promenade deck. Sections of the ship were converted to an operating room suite, an intensive-care ward, a specialized burn-care unit, and a “high dependency” skilled nursing unit, among other facilities. Over the ensuing campaign Uganda’s medical staff treated 730 casualties and performed 593 surgical procedures.
The liner Canberra was converted to a troop carrier with a major surgical facility. Original plans called for Canberra to receive casualties, although it did not qualify for Geneva Convention neutrality by virtue of having conveyed troops and equipment tothe theater. Unfortunately, after fierce attacks upon the fleet supporting the landing force, the British removed Canberra from the operational area, and elements of its medical organization were hurriedly put ashore at Ajax Bay.17
In addition, three ocean survey vessels were converted to Red Cross–identified ambulance ferry ships, which evacuated 593 casualties from Uganda to a neutral Red Cross–supervised aero-medical staging facility 420 miles away in Montevideo, Uruguay. From there they would be evacuated by air to Britain.18
Desert Shield/Desert Storm/Operation Granby (Great Britain)
Royal Navy casualty projections in the 1991 Persian Gulf campaign indicated the need for a minimum of a hundred beds in an afloat facility, able to admit mass casualties of all types, initiate their management, and hold them for six days. With no hospital ship then available, the Royal Navy designated the Royal Fleet Auxiliary’s air training ship RFA Argus to be that platform. Its flight deck, with five helicopter landing spots and two aircraft elevators, seemed ideal for movement of casualties. The British drew plans to convert the forward hangar to a hospital, in an airtight “subcitadel” (for chemical warfare protection). In three weeks the hospital had been designed, built, equipped, and staffed. Using modular construction techniques procured from a commercial vendor, the exoskeleton of the hospital was lifted to the flight deck in sections, lowered to the hangar deck, fitted together, and moved into position.19
Argus arrived in the Gulf with a hundred-bed hospital independent of the superstructure of the ship, including an intensive-care unit, a high-dependency skilled nursing unit, a low-dependency unit, four operating tables in two operating rooms with full support services, and a medical team of 136 men and women. The hospital was also supported by the ship’s air department, four Sea King helicopters designated for casualty evacuation, and Royal Navy support and liaison personnel. As a “grey hull” (a combatant in the eyes of international law), Argus could operate in forward areas with unrestricted communication, as ships with Geneva Convention neutrality protections cannot. This concept of afloat tactical medical support afforded significantly shortened casualty-transit time from frontline, at-risk naval units. Indeed, when a boiler exploded aboard the USS Iwo Jima (LPH 2) on 30 October 1990, a number of severely burned casualties were directly transferred to Argus for initial care.
Future Challenges
On 23 October 1983, a terrorist truck bomb carrying twelve thousand pounds of TNT detonated at the headquarters of the Marine Battalion Landing Team 1/8 at the Beirut, Lebanon, airport, killing 241 American servicemen and wounding 112. Sixty-two of the latter were sent to the offshore amphibious ship Iwo Jima, which had a surgical team. Several underwent surgery, and one died. A small group was subsequently sent to the British hospital in Akritori, Cyprus; fifty-six others were evacuated on a four-hour flight, during which an additional casualty died, to distant facilities in Landstuhl, Frankfurt, and Wiesbaden, Germany, as well as Naples, Italy (rather than those in neighboring Israel). As noted by a subsequent flag-level review, the only mass-casualty plan in place had involved Iwo Jima itself. There had been no effective coordinated theater plan for continuity of care, speedy evacuation, and regulation of victims of terrorist attacks—that is, allocation of each to the most capable treatment facility. As the review noted, “had the ratio of killed outright–to–wounded been reversed, so that over 200 casualties had required treatment, rather than fewer than 100, the medical system might well have failed.”20
Today, if a military force deployed from an offshore, dispersed, and geographically isolated strike group suffered a similar attack, a volume of instantaneously generated casualties of similar magnitude would require prompt and effective care. Any medical treatment system envisioned for geographically distributed operations must provide more timely and competent treatment and evacuation than was offered in Beirut. Given the unpredictable numbers of casualties produced by modern combat and the profound severity of survivable injuries inflicted by weaponry currently in use, it must be anticipated that existing forward facilities may be overwhelmed by “casualty overload.” Even over three decades ago, during the 1973 Yom Kippur War, an Israeli Defense Force evacuation hospital in the Sinai Desert, twenty to forty miles from the battle lines, received casualties in lots of from thirty-six to 140, and on one day 440. During the twenty-one days of fighting the facility treated 4,070 wounded, two-thirds of whom were in shock upon arrival.21
Distributed Expeditionary Sea Bases
Within a distributed sea-base context, a large volume of suddenly generated casualties could easily overwhelm the limited medical assets envisioned ashore. Furthermore, the improvised explosive devices used in the Middle East have shifted the spectrum of wounding. Advances in body armor and its wide deployment have diminished the incidence of mortal wounds of the chest and abdomen, but greater numbers of casualties with severe blast and fragmentary neurosurgical injuries to the head, brain, and neck, as well as major blood vessel (vascular) injuries of the extremities, may now survive long enough to reach forward combat unit medical staffs. They would ultimately be transported to a sea-based medical support center, if such were available.22
In the postulated sea-base medical continuum, the most rudimentary echelon of forward-located medical capabilities may be located at a battalion aid station (BAS), known as medical care Level I. During the Vietnam conflict, timely evacuation to such facilities was often assumed to be impractical, given delays and the occasional inaccessibility of aid stations due to “cantonment,” whereby troops lived in one location, were transported by helicopter to fight in another, and were then extracted—and so did not carry their bulky BAS with them. Sometimes medical aircraft evacuating severe injuries bypassed these limited lower-level facilities and flew directly to more advanced (Level II) surgical facilities capable of physician-assisted resuscitation, stabilization, and initial surgery to prolong life. There were also more specialized in-country facilities with subspecialty surgical capabilities, major blood-transfusion resources, and advanced levels of nursing support (Level III).
In the sea-base concept, the large-deck amphibious assault ships within the expeditionary strike groups (ESGs), of the LHA and LHD types, and presumably the forthcoming LHA replacement, the LHA(R), with Level II medical facilities and limited surgical capabilities for stabilizing injuries, will no doubt be the designated “casualty receiving and treatment ships.” Heretofore they have carried a standard Fleet Surgical Team augmentation of one general surgeon, an anesthesia provider, and other contingency medical and nursing augmentees. Facilities for Level III, or advanced specialty treatment, as has been available aboard T-AH hospital ships, will presumably be located elsewhere, perhaps in the Maritime Preposition Force (Future), or MPF(F), or in seagoing platforms provided by the other services. It has been suggested that newly designed ships for the MPF(F) will contain extensive medical-support modules with surgical specialty availability, allowing them to replace the aging hospital ships.23 These modules would require, however, specialized and trained surgical, anesthesia, and nursing personnel, triage and resuscitation space, equipment, and supplies matched to risks combatant personnel are being exposed to, presumably major blood-vessel injuries as well as life-threatening damage to the brain and spinal cord.
But the large-deck amphibious ships could in reality offer only limited surgical capabilities for stabilizing injuries. The primary mission of these ships is combat operations; the logistic, space, and mobility demands of casualty care cannot realistically be expected to outweigh the combat and combat-service imperatives. Further, despite the purported sixteen “intensive care” beds, the four surgical theaters of the LHA (and the six of the LHD), forty-seven ward beds (suspended from vertical chains), and many hundreds of “overflow beds” (if strike group personnel are off-loaded), space limitations result in the reality that ESG vessels are not supplied with sufficient casualty-support logistics for sustained treatment of large numbers of casualties. More importantly, they lack adequate numbers of the highly specialized medical and, especially, nursing personnel required by the wounds of blood vessels, brain, and spinal cord now being suffered in irregular and urban warfare.
For their part, the two current T-AH hospital ships, although well equipped and quite capable of advanced casualty care when adequately staffed with medical augmentees, are fading into operational obsolescence due to material aging, slow speed, and deep draft (which bars them from littoral waters).24 Nimitz-class nuclear aircraft carriers not only must primarily serve their operational roles but, in fact, are only marginally capable of in-depth care of multiple casualties, in terms of space, logistics, and personnel.
The LPD-17
The current amphibious fleet recapitalization plan involves the replacement of eleven smaller, aging amphibious landing ships, LPD-4s, and all twelve dock landing ships, LSDs, with new San Antonio–class LPD-17s. The new twenty-five-thousand-ton expeditionary warship—50 percent larger than the next-biggest LPD in the world—is designed to operate in an amphibious patrolling role twenty-five miles off a defended shore and in a nuclear environment. The ship is said to be capable of transporting seven hundred troops, with a surge capacity to eight hundred, and of receiving contaminated casualties through a specially designed triage center off the flight deck. It has two operating rooms, a twenty-four-bed ward, and a stated overflow capacity of one hundred casualties. The limits of its capabilities for combat injuries would be the breadth of available medical personnel and sufficient room available for handling a sudden large influx of casualties.
Limits would also arise from the huge space requirements of contingency medical logistic support. Combat casualties require large quantities of blood for transfusion, including fresh whole blood with clotting components (the latter is not found in either the LHA or LHD frozen blood repositories). During the Vietnam conflict, 10 percent of the wounded required blood replacement, the average being seven units per patient.25 Thirteen percent of those requiring blood required eleven or more units, some as many as ninety, most of which must be fresh blood with clotting components, to prevent further hemorrhaging. In addition, combat surgical staffs need wide-ranging capabilities not commonly found among surgical generalists, as well as twenty-four-hour availability of skilled nursing personnel and specific logistical support and resupply. Notwithstanding their seemingly advanced medical outfits, the San Antonio LPD and even the projected LSD(X) do not promise manifest, demonstrable value in the initial management of severe combat casualties. Their principal medical role might well be that of secondary casualty-reception facilities for wounded already treated and stabilized elsewhere.
The implications of such medical limitations were demonstrated during Operation URGENT FURY in October 1983, when the United States inserted forces into Grenada. In part because of an inadequately developed and insufficiently communicated joint medical support plan, Army helicopter pilots, unfamiliar with Navy ship profiles and flight decks, deposited critically injured personnel on the flight deck of USS Trenton (LPD 14), a ship with a designated “operating room” but minimal resources for critical care of casualties. One of these wounded, an Army ranger, was in shock due to massive blood loss from a wound through his chest and abdomen. With no blood bank, the general medical officers aboard Trenton were forced to match blood types with volunteer crew members using their identification tags alone, a highly irregular and potentially dangerous practice. They drew blood from the volunteers, literally on the spot, and transfused it warm directly into their critically injured patient before transferring him to the distant USS Guam (LPH 9), the largest medically capable ship in the operational area.26 Clearly, such older amphibious ships were inappropriate as primary casualty-reception sites.
Modularization
The Navy is analyzing ways to replace stand-alone systems through networking and modularity and to translate them into the basis for changes in the design of warships, at savings in both cost and risk. One such program is the Littoral Combat Ship. Its interchangeable, self-contained mission-specific modules, with standard interfaces to other modules and shipboard systems, could be swapped to meet various tactical needs—“plug and play.” New modules to support additional missions, such as emergency rescue and stability operations or environmental monitoring and support, would likely evolve as well.27
As noted, “medical modules” have also been proposed for employment as part of the MPF(F). The ships in this force will be kept in reduced operating status in strategic reserves around the world and activated as necessary. As we have also seen, a modular afloat medical facility (aboard RFA Argus) was successfully used by the British during the first Gulf War. Is this concept of providing robust medical support from the MPF(F) feasible?
Professional and paraprofessional personnel augmentees for MPF(F) modules would need to meet standards of care expected of land-based specialized surgical units and nursing facilities. Likewise, since burns constitute a substantial proportion of wounds inflicted in naval warfare (in the Falklands campaign, 33 percent of the wounds treated in the hospital ship Uganda were burns) ample accommodation must be made for them (as well as for management of patients with blood vessel and neurological injuries).28 Since these modules would lie in reduced operating status until mobilized, their functional status will require systematic monitoring, their perishable supplies tied to “just in time delivery arrangements” wherever MPF(F) ships are maintained, and their professional staffs identified, funded, and trained to function in that environment.
Missions for the Future
As currently envisioned, the squadron configuration selected for the Navy’s Maritime Prepositioned Force (Future) will consist of fourteen ships: twelve new-construction hulls and two existing T-AKR “dense-packed” ships carrying supplies and ammunition. The twelve new ships will be: two T-LHA(R)s, equipped with command and control facilities for a Marine expeditionary brigade; one T-LHD with aviation command-and-control facilities; three modified large, medium-speed, roll-on/roll-off (LMSR) sealift ships; three modified Lewis and Clark–class (T-AKE 1) cargo and ammunition resupply ships; and three mobile landing-platform-type vessels capable of housing 1,100 troops each. These latter innovative vessels should be capable of meeting surface assault requirements without external or aviation support by partially submerging and allowing cargo to float on and off to connector ships.29 It is anticipated that since the LHA(R)s and LHDs will be conducting forcible-entry and other belligerent operations, they will require reclassification as warships when activated and undergo augmentation by Navy crews. The others will operate, when activated, under the aegis of the Military Sealift Command and be manned by civilian mariners.
From a medical perspective, the first question to be asked, then, is: What are command expectations for the medical assets functioning in a joint sea-base environment? The follow-on questions are: What resources will be necessary to enable the joint/combined-force casualties to reach competent medical facilities within the sea base in a timely manner? In what form will these facilities exist? The answers will not only drive the activity of planners but will ultimately allow more realistic implementation on site during conflict.
The bulk of casualties ashore would be evacuated to the sea base by air, and when required by high-speed, seagoing “connector” vessels. (The LHA[Rs will have no well decks; casualties will have to reach them exclusively by air, or by other as-yet-unproven innovative methods. This may be particularly important during times when weather is too foul for vertical transport. Alternatives such as waterline access or loading platforms alongside may be required). The connectors envisioned (for lift within the sea base as well as long distance) include the Joint High Speed Vessel, the V-22 Osprey, and the CH-53K heavy-lift helicopter. In 2004 the Navy Warfare Development Command conducted an experiment to evaluate the High Speed Vessel as a medical platform. Unfortunately, it found, surgical interventions on board were precluded by high ambient vibration, noise levels, and vessel motion (including severe pounding) at high speeds or sea states—aside from motion sickness of both patients and staff.30 These findings might clearly impact upon survivability during long-range transport aboard such vessels.
If the ships of the sea base are to be kept continuously available for new incoming casualties without overload, initially treated and stabilized casualties need to be systematically forwarded to higher-level medical facilities, perhaps thousands of miles away. This will require creativity, such as displayed by the British at the Falklands, who used converted ocean survey ships as seagoing ambulances.31
Joint Operations: The Need For Integration and Accommodation
Unfortunately, a recent Government Accountability Office (GAO) report on sea basing has identified a lack of “unifying vision” within the defense community with regard to sea-base development.32 It notes that individual services appear to be outpacing the Defense Department. For example, the Army is developing its own Joint High Speed Vessel and Joint High Speed Sealift Ship programs. Furthermore, the Army is also beginning to develop its own Afloat Forward Staging Base, intended to provide aerial maneuver for Army forces “from the sea.” One option being explored is adding flight decks to commercial containerships.33
The inevitable result of such independent activity, however, is the potential for redundancy and a lack of joint coordination, medical support not excepted.
In the absence of an overarching joint experimentation campaign plan, indicates the GAO, many sea-basing investigations—including war gaming, operations analysis, workshops, technological development, modeling and simulation, platform prototyping, and live demonstrations—have taken place across the services, combatant commands, and other defense entities, without the ability to evaluate solutions, including medical considerations, or to coordinate efforts. Likewise, notes the report, there are insufficient modeling and simulation tools available. All this will clearly impact upon doctrine and training as well as any concrete solutions that may be proposed for dealing with the combat wounded. Ultimately, the Navy must coordinate with other services on stable standards for a truly joint and interoperable medical support network.
The Bottom Line
The distributed sea base is to be composed of a series of complex platforms, connectors, and logistics technologies. Logically, it must be driven by a common set of standards, requirements, time frames, and priorities. The advent of the integrated base at sea requires adaptive medical systems “engineering” as well. Within that metaphor, configuration management will be extremely important to ensure connectivity among systems and components—in fact, a “system of systems” approach—for both technical support and logistics.34 Various ship, airlift, and sealift components for casualty evacuation and treatment will need to interface, and some of them will have to be interdependent. In addition, joint operations from a sea base will require robust logistics technologies, as well as command and control. Premature development of such systems to meet individual service requirements for medical support rather than joint necessities may facilitate initiatives that are duplicative, not interoperable, and possibly incompatible. Ultimately, adverse consequences for combat casualties may result.
The fundamental “bottom line” in any assessment of casualty care, whether single service, joint, or combined, relates to time expended in transporting a wounded person to a proper setting where a constructive medical intervention can be performed. This must dominate every discussion of support systems. (Delay in access to adequate care implies a precipitous decline into the ominous “Triangle of Death,” which correlates with entry into an irreversible downward spiral from which there is commonly no return to normal health.) Neglect of this very specific requirement translates into acceptance by operational commanders of increased mortality and morbidity among accrued casualties.
A casual observer visiting a large deck amphibious ship may well be overwhelmed with the abundance of equipment and space available to serve the wounded. Deeper evaluation, however, will reveal that the mere availability of equipment on a sea base ship will not, in itself, insure the availability of the requisite care needed by large numbers of combat wounded. The thrust of any analysis of medical support at sea must emphasize the importance of the time factor, as well as reference to previous empirical adaptations that have been implemented to address the “time to receipt of substantive treatment” issue in various operational theaters.
In conjunction with new and evolving operational approaches that emphasize joint and combined operations, a medical support system and its component material parts must be designed to supply speed, flexibility, and, above all, responsiveness. The corollary is that logistical support, including medical services, must always be adaptive. It must be capable of responding to the unique nature of the conflict in hand and to the operational concepts employed by combatant commanders. In the current context, casualty care must be adapted to geographically dispersed, or “distributed,” sea-based operations in the littorals, with minimal medical facilities ashore.
A harmonious vision of sea-based medical support, supported by pragmatic leadership, is an absolute prerequisite to rapid and effective time-sensitive care for the combat wounded during the unpredictable but probably inevitable littoral conflicts of the future.