Abstract
Background
The Australian Department of Defence commissioned a scoping review and catalogue of research investigating the health of Australian Defence Force (ADF) members, published between 2002 and 2023.
Material and methods
MEDLINE, Embase, PsycINFO, Cochrane Central Register of Controlled Trials and Web of Science databases were searched in April 2023 for peer-reviewed studies published since 2002. Eligibility criteria included studies that involved ADF personnel (serving or transitioning at the time of the study intervention), health and wellbeing outcomes (other than malaria), and English-language publications. Data were extracted using a template developed by the authors, and risk of bias was assessed using the JBI Institute critical appraisal tools. Studies were categorised according to the eight strategic health priorities identified by the Australian Department of Defence.
Results
The database searches identified 171 peer-reviewed studies. Most were either cohort (n=71; 41%) or cross-sectional (n=45; 26%) in design. Fourteen (8%) studies were randomised trials. The health research areas most frequently addressed were mental health (n=78; 47%), musculoskeletal (n=46; 27%), and occupational and environmental exposure (n=23; 13%). The Department of Defence or Department of Veterans’ Affairs funded 74% of studies. A further 60 reports (provided by the Department or retrieved through grey literature) were included in the evidence catalogue and reflected the same common research areas.
Conclusion
The evidence synthesis catalogue provides an overview of the range of research investigating the health of ADF personnel since 2002. Cataloguing past health research has provided insights into the importance of aligning research focus with ADF priorities. It provides an opportunity to consider strategies to ensure that future health research aligns closely with ADF priorities.
Keywords: military health, Australian Defence Force, musculoskeletal, mental health, occupational health
Introduction
The Australian Defence Force (ADF) is one of the largest employers in Australia; in 2021/2022, there were 58 342 permanent ADF members and approximately 21 500 Reserve members in a diverse range of job roles.1 The ADF exists to defend Australia and its national interests and to be an advocate for stability, security and sovereignty in the Indo-Pacific region. As with all armed forces, the ADF recruits ‘healthy workers’2,3 capable of being trained to be part of Australia’s response to the spectrum of conflict, which includes the use of credible force when required, peacekeeping, humanitarian and disaster relief, and domestic operations. In August 2023, the ADF Health Strategy4 was released to ensure that the Defence health system continues to deliver world-class healthcare while evolving to meet the needs of the future force. Within the ADF Health Strategy, a key enabler is described as a ‘unified, targeted and timely approach to research with feedback mechanisms to Defence planning processes’.5 The Defence Health Research Framework (2021–2025) also highlights the aim to ‘build and strengthen pathways for translating research findings into policy and practice’.5 The World Health Organization (WHO) defines knowledge translation as the ‘synthesis, exchange, and application of knowledge by relevant stakeholders to accelerate the benefits of global and local innovation in strengthening health systems and improving people’s health’.6
To progress the ADF Health Strategy, the Department of Defence commissioned the Monash Centre for Occupational and Environmental Health to conduct a scoping review and synthesis of health research findings from 2002 to 2023, and to catalogue the research according to the eight health research priority themes. These priority areas were developed in 2022, following an examination of available evidence, stakeholder input and available data on the health of the force, and included: 1) Measuring and monitoring the health of the force; 2) Health of the future warfighter; 3) Musculoskeletal injuries; 4) Occupational and environmental health; 5) Mental health and wellbeing; 6) Health system performance and efficiency; 7) Gender and health; and 8) Infectious disease. The aim was to catalogue all research investigating the health of ADF members (excluding malaria research, as the Australian Defence Force Malaria and Infectious Disease Institute oversees malaria research) conducted and published over the previous 20 years, along with a risk-of-bias assessment. This activity would support the implementation of the ADF Health Research Framework 2021–2025.
Method
The protocol for this study was developed by the authors in consultation with the Department of Defence and informed by the PRISMA-ScR (Preferred Reporting Items for Systematic Reviews and Meta-Analysis—Scoping Reviews) guidelines.7 Since this study is primarily a scoping review of publications relating to a single country (with synthesis of a subset of studies), the project does not meet the criteria for a systematic review required for registration in PROSPERO. However, three related specific topic reviews were registered in International Platform of Registered Systematic Review and meta- analysis Protocols (INPLASY) (registration numbers INPLASY202420076 (Post-traumatic stress disorder in Australian Defence Personnel 2002–23: A systematic review of incidence, prevalence, risk factors and treatment); INPLASY202420077 (Gender and health in ADF personnel 2002-2023: A systematic review and synthesis); and INPLASY202420078 (Affective disorders including depression in ADF personnel 2002–2023: A systematic review of incidence, prevalence and risk factors).
Eligibility criteria
The eligibility criteria for the studies were devised using the PICO framework.8 Studies were included if they met the following criteria: 1) participants were current serving Permanent and Reserve ADF members or ADF members in transition (transferring from the ADF to civilian life), and 2) the study measured outcomes that were focused on health or wellbeing. All study design types were included. Studies of former serving ADF members, families and children of serving ADF members, and non-Australian military personnel were out of scope for this review. Additionally, studies were not included if they related to malaria, if data about current serving ADF members were not presented separately from former serving ADF members, or if they were opinion pieces, narrative reviews or commentaries.
Search methods
The search was developed by an information specialist (SM), with input from subject matter experts. Searches combined subject headings and free-text terms related to the military and military health with the subject heading and text word Australia (Table S1, supplementary material).
Table S1. Database search strategies for the ADF Catalogue 2002–2023
MEDLINE
Ovid MEDLINE ALL 1946 to 21 April 2023
| # | Search statement | Results |
| 1 | (Military Personnel/ or Military Health/ or exp Naval Medicine/ or Military Family/ or Psychology, Military/ or Military Psychiatry/ or (Military Medicine/ not historical article.pt.)) and (exp Australia/ or Australia*.ti,ab,kf.) | 666 |
| 2 | ((defence or defense or military* or army or armies or armed or combat or soldier* or troop* or infantry or air force or RAAF or fighter pilot* or navy or naval or sailor* or submariner* or active dut* or service personnel or servicewomen or servicemen or regiment* or squadron* or battalion* or coastguard* or coast guard*) adj20 Australia*).ti,ab,kf. | 901 |
| 3 | (defence or defense or military* or army or armies or armed or combat or soldier* or troop* or infantry or air force or RAAF or fighter pilot* or navy or naval or sailor* or submariner* or active dut* or service personnel or servicewomen or servicemen or regiment* or squadron* or battalion* or coastguard* or coast guard*).ti,ab,kf. and (Australian Defence Force or (department of defence adj3 Australia*)).in. | 95 |
| 4 | or/1-3 | 1241 |
| 5 | limit 4 to yr=”2002 -Current” | 847 |
Embase
Ovid Embase Classic + Embase 1947 to 21 April 2023
| # | Search statement | Results |
| 1 | (exp Military Personnel/ or Military Health/ or Military Health Service/ or exp Military Family/ or (Military Medicine/ not History/)) and (exp Australia/ or australia*.ti,ab,kf.) | 238 |
| 2 | ((defence or defense or military* or army or armies or armed or combat or soldier* or troop* or infantry or air force or RAAF or fighter pilot* or navy or naval or sailor* or submariner* or active dut* or service personnel or regiment* or squadron* or battalion* or coastguard* or coast guard*) adj20 Australia*).ti,ab,kf. | 1139 |
| 3 | (defence or defense or military* or army or armies or armed or combat or soldier* or troop* or infantry or air force or RAAF or fighter pilot* or navy or naval or sailor* or submariner* or active dut* or service personnel or regiment* or squadron* or battalion* or coastguard* or coast guard*).ti,ab,kf. and (Australian Defence Force or (department of defence adj3 Australia*)).in. | 146 |
| 4 | or/1-3 | 1307 |
| 5 | exp Animal/ not exp Human/ | 5954285 |
| 6 | 4 not 5 | 1235 |
| 7 | limit 4 to yr=”2002 -Current” | 946 |
CENTRAL
Cochrane Central Register of Controlled Trials (Cochrane Library, Issue 3, 2023)
| # | Search statement | Results |
| 1 | (Military Personnel/ or Military Health/ or exp Naval Medicine/ or Military Family/ or Psychology, Military/ or Military Psychiatry/ or Military Medicine/) and (exp Australia/ or Australia*.af.) | 51 |
| 2 | ((defence or defense or military* or army or armies or armed or combat or soldier* or troop* or infantry or air force or RAAF or fighter pilot* or navy or naval or sailor* or submariner* or active dut* or service personnel or regiment* or squadron* or battalion* or coastguard* or coast guard*) adj20 Australia*).af. | 146 |
| 3 | or/1-2 | 153 |
| 4 | limit 3 to yr=”2002 -Current” | 131 |
PsycINFO
Ovid APA PsycINFO 1806 to Week 3 April 2023
| # | Search statement | Results |
| 1 | (exp Military Personnel/ or Military Psychiatry/ or Military Psychology/ or Military Families/) and Australia*.mp. | 384 |
| 2 | ((defence or defense or military* or army or armies or armed or combat or soldier* or troop* or infantry or air force or RAAF or fighter pilot* or navy or naval or sailor* or submariner* or active dut* or service personnel or regiment* or squadron* or battalion* or coastguard* or coast guard*) adj5 Australia*).mp. | 576 |
| 3 | (defence or defense or military* or army or armies or armed or combat or soldier* or troop* or infantry or air force or RAAF or fighter pilot* or navy or naval or sailor* or submariner* or active dut* or service personnel or regiment* or squadron* or battalion* or coastguard* or coast guard*).mp. and (Australian Defence Force or (department of defence adj3 Australia*)).in. | 34 |
| 4 | or/1-3 | 702 |
| 5 | limit 4 to yr=”2002 -Current” | 510 |
Web of Science Core Collection
24 April 2023
AB=((Australian defence or Australian defense or Australian military or Australian armed or Australian army or Australian soldier* or Australian troop* or Australian air force or Australian navy or Australian naval or Australian sailor* or Australian submariner* or Australian combat))
Limited to WoS categories: Medicine General Internal; Public Environmental Occupational Health; Psychiatry; Rehabilitation
PY 2002-2022 = 649
The search was conducted on 24 April 2023 and was limited to studies published after 1 January 2002. Five electronic databases were searched: Web of Science Core Collection, Medline, Embase, PsycINFO and the Cochrane Central Register of Controlled Trials. The ProQuest Military Database was initially included; however, only a few studies identified in this database were health-related and were subsequently duplicated in Medline. Consequently, ProQuest Military Database was removed from the search. Bibliographies of included studies were checked to identify any additional relevant studies.
The Department of Defence provided internal publicly available research reports that investigated or reported on health outcomes. In addition, a search of grey literature for additional research reports and theses was conducted on the websites of known related research institutions.
Study selection
Retrieved records were imported into EndNote, de-duplicated and then added to Covidence software. Approximately 20% of records were independently screened at the title/abstract level by two reviewers (HK, KWB) to establish reviewer consistency, using a pre-established strategy developed by the screening team. Conflicts were resolved by consensus. The remaining records were screened by one reviewer (HK). Three reviewers screened potential studies at the full-text level (HK, KWB, NK). Any discrepancies were resolved through discussion.
Outcome measures
Eligible outcome measures were any health or wellbeing-related outcomes, except for studies that investigated/reported only malaria, studies that focused only on aspects of performance (e.g., fitness levels) and studies that included only validation of health-related metrics. Studies on malaria were excluded, as the Australian Defence Force Malaria and Infectious Disease Institute oversees malaria health research.
Risk of bias
Risk of bias was assessed for each included study. The following JBI critical appraisal tools were used: Checklist for Analytical Cross-Sectional Studies, Checklist for Case Control studies, Checklist for Case Reports, Checklist for Cohort Studies, Checklist for Diagnostic Test Accuracy Studies, Checklist for Prevalence Studies, Checklist for Quasi-Experimental Appraisal Tool, Checklist for Systematic Review and Research Syntheses, and Checklist for Randomised Control Trials (RCTs) (https://jbi.global/critical-appraisal-tools).
An overall risk-of-bias rating (low, moderate or high) was assigned to each study. Consistent with best-practice guidelines,9 the judgement was based on weighting the assessment of critical domains, rather than a checklist or scoring framework. Consequently, some studies with an overall rating of high risk of bias may have had only one high-risk critical domain, while others may have had multiple unclear critical domains. Determining whether a domain was critical depended on the study’s context. Consequently, the designation of ‘critical’ to a domain varied between studies. For RCTs, the domain of ‘blinding of participants’ was assessed; however, since blinding participants is invariably difficult to achieve in occupational intervention studies, non-blinding was not considered a critical domain in deriving an overall rating for these studies. An ‘unclear’ assessment was made for domains that could not be fully assessed due to incomplete information in the publication.
Each study was independently assessed by two authors who were not co-authors of that publication, with any disagreements resolved through discussion. A third author arbitrated if consensus could not be reached.
Data extraction
The authors devised a data extraction form. Three authors independently extracted data from five studies to assess the consistency and applicability of the form. Slight adjustments were then made to the form, with the final categories being: study type, participant details, intervention/exposure, comparator, outcome, health domain, inclusion and exclusion criteria and findings. A single author extracted data for each of the remaining studies. A senior member of the research team (KWB) conducted a second data extraction of 5% of the studies to verify accuracy. Data were entered into an Excel spreadsheet, with a separate column for each data variable. The data extraction table for the reports included an additional column detailing related studies derived from each report.
Development of the evidence catalogue
For each study, information was extracted to define which specific health outcomes had been evaluated and reported, so that each study could be catalogued into the most applicable health research priority area. An additional category, ‘other health outcome’, was created for studies that did not meet the criteria for any of the eight specified priority health research areas. Some studies included multiple health outcomes; these studies were catalogued under a maximum of three health research priority areas for ease of use.
Results
Study selection
A total of 3083 records were retrieved through the database search (Figure 1). After removal of 1201 duplicates, 1882 records were screened at the title/abstract level, of which 1522 were excluded. After full-text screening, 195 studies were excluded and 165 studies were included. A further six studies were included after a search of the bibliographies of included studies (Figure 1). A small number of the included studies (n=5) focused on former serving ADF members who were serving at the time of exposure (deployment)— Defence deemed these studies to have a particularly valuable contribution to the health research evidence catalogue. This resulted in a total of 171 studies for inclusion (Table S2, supplementary material).
Table S2: Bibliographic details of 171 papers included in the ADF evidence catalogue 2002–2023
| Study |
| Abouzeid M, Kelsall HL, Forbes AB, et al. Posttraumatic stress disorder and hypertension in Australian veterans of the 1991 Gulf War. J Psychosom Res. 2012;72(1):33-38. |
| Aidman E, Jackson SA, Kleitman S. Effects of sleep deprivation on executive functioning, cognitive abilities, metacognitive confidence, and decision making. Appl Cogn Psychol. 2019;33(2):188-200. doi:https://dx.doi.org/10.1002/acp.3463 |
| Alele FO, Malau-Aduli BS, Malau-Aduli AEO, et al. Individual anthropometric, aerobic capacity and demographic characteristics as predictors of heat intolerance in military populations. Medicina (Kaunas). 2021;57(2):173. |
| Arthur DTJ, Khan MM, Barclay LC. Thermographic investigation of osseous stress pathology. Annual International Conference of the IEEE Engineering in Medicine and Biology Society IEEE Engineering in Medicine and Biology Society Annual International Conference. 2011;2011:6250-6253. |
| Attia JR, D’Este C, Schofield PW, et al. on behalf of the SHOAMP Team. Mental health in F-111 maintenance workers: the study of health outcomes in aircraft maintenance personnel (SHOAMP) general health and medical study. J Occup Environ Med. 2006;48:682-691. |
| Barton CA, McGuire A, Waller M, et al. Smoking prevalence, its determinants and short-term health implications in the Australian Defence Force. Mil Med. 2010;175(4):267-272. |
| Bleier J, McFarlane A, McGuire A, et al. Risk of adverse health outcomes associated with frequency and duration of deployment with the Australian Defence Force. Mil Med. 2011;176(2):139-146. |
| Bonanno D, Murley G, Munteanu S, et al. Effectiveness of foot orthoses for the prevention of lower limb overuse injuries in naval recruits: a randomised controlled trial. Br J Sports Med. 2018;52(5):298-302. |
| Bonanno DR, Munteanu SE, Murley GS, et al. Risk factors for lower limb injuries during initial naval training: a prospective study. J R Army Med Corps. 2018;164(5):347-351. |
| Booth CK, Coad RA, Forbes-Ewan CH, et al. The physiological and psychological effects of combat ration feeding during a 12-day training exercise in the tropics. Mil Med. 2003;168(1):63-70. |
| Booth CK, Probert B, Forbes-Ewan C, et al. Australian army recruits in training display symptoms of overtraining. Mil Med. 2006;171(11):1059-1064. |
| Brown A, Gibson R, Tavener M, et al. Sexual function in F-111 maintenance workers: the study of health outcomes in aircraft maintenance personnel. J Sex Med. 2009;6(6):1569-1578. |
| Bull C, Ellwood D, Toohill J, et al. Quantifying the differences in birth outcomes and out-of-pocket costs between Australian Defence Force servicewomen and civilian women: a data linkage study. Women Birth. 2022;35(5):e432-e438. |
| Burley SD, Drain JR, Sampson JA, et al. Effect of a novel low volume, high intensity concurrent training regimen on recruit fitness and resilience. J Sci Med Sport. 2020;23(10):979-984. |
| Burne SG, Khan KM, Boudville PB, et al. Risk factors associated with exertional medial tibial pain: a 12 month prospective clinical study. Br J Sports Med. 2004;38(4):441-445. |
| Burnett AF, Naumann FL, Burton EJ. Flight-training effect on the cervical muscle strength of trainee pilots. Aviat Space Environ Med. 2004;75(7):611-615. |
| Cable GG. In-flight hypoxia incidents in military aircraft: causes and implications for training. Aviat Space Environ Med. 2003;74(2):169-172. |
| Cash R, Varker T, McHugh T, et al. Effectiveness of an anger intervention for military members with PTSD: A clinical case series. Mil Med. 2018;183(9-10):e286-e290. |
| Cohn A, Pakenham K. Efficacy of a cognitive-behavioral program to improve psychological adjustment among soldiers in recruit training. Mil Med. 2008;173(12):1151-1157. |
| Colgrave N. Special operations task group regimental aid post presentations, Tarin Kowt, Afghanistan: February – June 2010. J Mil Veterans Health. 2011;19(3):13-19. |
| Coltman CE, Steele JR, Spratford WA, et al. Are female soldiers satisfied with the fit and function of body armour? Appl Ergon. 2020;89:103197. |
| Coltman CE, Brisbine BR, Molloy RH, et al. Identifying problems that female soldiers experience with current-issue body armour. Appl Ergon. 2021;94:103384. |
| Cowlishaw S, Metcalf O, Lawrence-Wood E, et al. Gambling problems among military personnel after deployment. J Psychiatr Res. 2020;131:47-53. |
| Cowlishaw S, Metcalf O, Little J, et al. Cross-lagged analyses of anger and PTSD symptoms among veterans in treatment. Psychol Trauma. 2022;14(2):336-345. |
| Crane MF, Boga D, Karin E, et al. Strengthening resilience in military officer cadets: A group-randomized controlled trial of coping and emotion regulatory self-reflection training. J Consult Clin Psychol. 2019;87(2):125-140. |
| Crane MF, Forbes D, Lewis V, et al. The interplay between social interaction quality and wellbeing in military personnel during their initial two-years of service. Mil Psychol. 2022;34(5):503-515. |
| Creamer M, Carboon I, Forbes AB, et al. Psychiatric disorder and separation from military service: a 10-year retrospective study. Am J Psychiatry. 2006;163(4):733-734. |
| Crocombe LA, Mahoney GD, Spencer AJ, et al. Will improving access to dental care improve oral health-related quality of life? Aust Dent J. 2013;58(2):192-199. |
| Crocombe LA, Mahoney GD. Does optimal access to dental care counteract the oral health-related quality of life social gradient? Aust Dent J. 2016;61(4):418-424. |
| Davy CP, Lorimer M, McFarlane A, et al. The well-being of Australian service mothers. Women Health. 2015;55(7):737-753. |
| Dawson GME, Broad R, Orr RM. The impact of a lengthened Australian Army recruit training course on recruit injuries. J Mil Veterans Health. 2015;23(2):14-19. |
| Dell L, Casetta C, Benassi H, et al. Mental health across the early years in the military. Psychol Med. 2022:1-9. |
| Dell L, Sbisa AM, Forbes A, et al. Massed v. standard prolonged exposure therapy for PTSD in military personnel and veterans: 12-month follow-up of a non-inferiority randomised controlled trial. Psychol Med. 2023:1-8. |
| Dell L, Sbisa AM, Forbes A, et al. Effect of massed v. standard prolonged exposure therapy on PTSD in military personnel and veterans: a non-inferiority randomised controlled trial. Psychol Med.2022:1-8. |
| D’Este C, Attia JR, Brown AM, et al. Cancer incidence and mortality in aircraft maintenance workers. Am J Ind Med. 2008;51(1):16-23. |
| Esterman A, Pilotto L. Foot shape and its effect on functioning in Royal Australian Air Force recruits. Part 1: Prospective cohort study. Mil Med. 2005;170(7):623-628. |
| Esterman A, Pilotto L. Foot shape and its effect on functioning in Royal Australian Air Force recruits. Part 2: Pilot, randomized, controlled trial of orthotics in recruits with flat feet. Mil Med. 2005;170(7):629-33. |
| Falon SL, Karin E, Boga D, et al. A clustered-randomized controlled trial of a self-reflection resilience-strengthening intervention and novel mediators. J Occup Health Psychol. 2021;26(1):1-19. |
| Forbes AB, McKenzie DP, Mackinnon AJ, et al. The health of Australian veterans of the 1991 Gulf War: factor analysis of self-reported symptoms. Occup Environ Med. 2004;61(12):1014-1020. |
| Forbes D, Bennett N, Biddle D, et al. Clinical presentations and treatment outcomes of peacekeeper veterans with PTSD: preliminary findings. Am J Psychiatry. 2005;162(11):2188-2190. |
| Forbes D, O’Donnell M, Brand RM, et al. The long-term mental health impact of peacekeeping: prevalence and predictors of psychiatric disorder. BJPsych Open. 2016;2(1):32-37. |
| Fuente A, Hickson L, Morata TC, et al. Jet fuel exposure and auditory outcomes in Australian air force personnel. BMC Public Health. 2019;19(1):675. |
| Garnock C, Witchalls J, Newman P. Predicting individual risk for medial tibial stress syndrome in navy recruits. J Sci Med Sport. 2018;21(6): 586-590. |
| Gibson N, Drain JR, Larsen P, et al. A comprehensive analysis of injuries during army basic military training. Mil Med. 2022;1:1-9. |
| Goodall RL, Pope RP, Coyle JA, et al. Balance and agility training does not always decrease lower limb injury risks: a cluster-randomised controlled trial. Int J Inj Contr Saf Promot. 2013;20(3):271-281. |
| Graham K, Searle A, Van Hooff M, et al. The associations between physical and psychological symptoms and traumatic military deployment exposures. J Trauma Stress. 2019;32(6):957-966. |
| Graham K, Searle A, Van Hooff M, et al. The value of physical symptoms in screening for posttraumatic stress disorder in the military. Assessment. 2020;27(6):1139-1150. |
| Graham K, Lawrence-Wood E, McFarlane A. Longitudinal relationship between posttraumatic stress symptoms and physical symptoms in military veterans. Psychosom Med. 2022;84(9):1034-1040. |
| Gucciardi DF, Lang JWB, Lines RLJ, et al. The emergence of resilience: Recovery trajectories in sleep functioning after a major stressor. Sport Exerc Perform Psychol. 2021;10(4):571-589. |
| Guest M, Boggess M, Attia J, et al. Hearing impairment in F-111 maintenance workers: the study of health outcomes in aircraft maintenance personnel (SHOAMP) general health and medical study. Am J Ind Med. 2010;53(11):1159-1169. |
| Guest M, Attia JR, D’Este CA, et al. Peripheral neuropathy in military aircraft maintenance workers in Australia. J Occup Environ Med. 2011;53(4):381-387. |
| Guest M, D’Este C, Attia J, et al. Impairment of color vision in aircraft maintenance workers. Int Arch Occup Environ Health. 2011;84(7):723-733. |
| Guest M, Boggess M, Attia J. Relative risk of elevated hearing threshold compared to ISO1999 normative populations for Royal Australian Air Force male personnel. Hear Res. 2012;285(1-2):65-76. |
| Gwini SM, Forbes AB, Kelsall HL, et al. Increased symptom reporting persists in 1990–1991 Gulf War Veterans 20 years post deployment. Am J Ind Med. 2015:58:1246–1254. |
| Gwini SM, Forbes AB, Sim MR, et al. Multisymptom illness in Gulf War veterans: A systematic review and meta-analysis. J Occup Environ Med. 2016;58(7):659-667. |
| Gwini SM, Kelsall HL, Sim MR, Ikin JF, McFarlane AC, Forbes AB. Stability of symptom patterns in Australian Gulf War veterans: 10-year longitudinal study. Occup Environ Med. 2016;73(3):195-198. |
| Gwini SM, Forbes AB, Sim MR, et al. Comparability of health service use by veterans with multisymptom illness and those with chronic diseases. Int J Qual Health Care. 2017;29(1):90-97. |
| Hansen C, McFarlane A, Iannos M, et al. Psychosocial factors associated with psychological distress and functional difficulties in recently transitioned and current serving regular Australian Defence Force members. Psychiatry Res. 2020;286:112860. |
| Hopcraft M, Morgan M. Dental caries experience in a young adult military population. Aust Dent J. 2003;48(2):125-129. |
| Hopcraft MS, Morgan MV. Exposure to fluoridated drinking water and dental caries experience in Australian army recruits, 1996. Community Dent Oral Epidemiol. 2003;31(1):68-74. |
| Hopcraft M, Morgan MV. Dental caries experience in Australian Army recruits 2002-2003. Aust Dent J. 2005;50(1):16-20. |
| Hopcraft MS, Yapp KE, Mahoney G, et al. Dental caries experience in young Australian Army recruits 2008. Aust Dent J. 2009;54(4):316-322. |
| Howard A, Agathos JA, Phelps A, et al. Prevalence and treatment implications of ICD-11 complex PTSD in Australian treatment-seeking current and ex-serving military members. Eur J Psychotraumatol. 2021;12(1):1844441. |
| Hughes CD, Weinrauch PCL. Military static line parachute injuries in an Australian commando battalion. ANZ J Surg. 2008;78(10):848-852. |
| Hunt AP, Billing DC, Patterson MJ, Caldwell JN. Heat strain during military training activities: The dilemma of balancing force protection and operational capability. Temperature (Austin). 2016;3(2):307-317. |
| Hunt AP, Stewart IB, Billing DC. Indices of physiological strain for firefighters of the Australian Defence Forces. J Occup Environ Hyg. 2019;16(11):727-734. |
| Ikin JF, Sim MR, Creamer MC, et al. War-related psychological stressors and risk of psychological disorders in Australian veterans of the 1991 Gulf War. Br J Psychiatry. 2004;185:116-126. |
| Ikin JF, McKenzie DP, Gwini SM, et al. Major depression and depressive symptoms in Australian Gulf War veterans 20 years after the Gulf War. J Affect Disord. 2016;189:77-84. |
| Ikin JF, Kelsall HL, McKenzie DP, et al. Cohort Profile: The Australian Gulf War Veterans’ Health Study cohort. Int J Epidemiol. 2017;46(1):31. |
| Ireland R, Waller M, MacKenzie A, et al. Assessment of revised recruitment standards for asthma in the Australian Defence Force. Mil Med. 2014;179(11):1384-1390. |
| Kanesarajah J, Waller M, Zheng WY, et al. Unit cohesion, traumatic exposure and mental health of military personnel. Occup Med (Lond). 2016;66(4):308-315. |
| Kelsall HL, Sim MR, Forbes AB, et al. Symptoms and medical conditions in Australian veterans of the 1991 Gulf War: relation to immunisations and other Gulf War exposures. Occup Environ Med. 2004;61(12):1006-1013. |
| Kelsall HL, Sim MR, Forbes AB, et al. Respiratory health status of Australian veterans of the 1991 Gulf War and the effects of exposure to oil fire smoke and dust storms. Thorax. 2004;59(10):897-903. |
| Kelsall H, Macdonell R, Sim M, et al. Neurological status of Australian veterans of the 1991 Gulf War and the effect of medical and chemical exposures. Int J Epidemiol. 2005;34(4):810-819. |
| Kelsall H, Sim M, McKenzie D, et al. Medically evaluated psychological and physical health of Australian Gulf War veterans with chronic fatigue. J Psychosom Res. 2006;60(6):575-84. |
| Kelsall HL, Sim MR, Ikin JF, et al. Reproductive health of male Australian veterans of the 1991 Gulf War. BMC Public Health. 2007;7:79. |
| Kelsall H, McKenzie D, Sim M, et al. Comparison of self-reported and recorded vaccinations and health effects in Australian Gulf War veterans. Vaccine. 2008;26(33):4290-4297. |
| Kelsall HL, McKenzie DP, Sim MR, et al. Physical, psychological, and functional comorbidities of multisymptom illness in Australian male veterans of the 1991 Gulf War. Am J Epidemiol. 2009;170(8):1048-1056. |
| Kelsall HL, McKenzie DP, Forbes AB, et al. Pain-related musculoskeletal disorders, psychological comorbidity, and the relationship with physical and mental well-being in Gulf War veterans. Pain. 2014;155(4):685-692. |
| Kirk KM, McGuire A, Nielsen L, et al. Self-reported tinnitus and ototoxic exposures among deployed Australian Defence Force personnel. Mil Med. 2011;176(4):461-467. |
| Kirk KM, McGuire A, Nasveld PE, et al. Comparison of self-reported and audiometrically-measured hearing loss in the Australian Defence Force. Int J Audiol. 2012;51(4):294-298. |
| Kitchener S. Ultraviolet radiation exposure and melanoma in Australian naval personnel (Reprinted from Aust Mil Med. 2001;10:55-59. J Mil Veterans Health. 2011;19(3):50-54. |
| Lenton GK, Doyle TLA, Saxby DJ, et al. Integrating a hip belt with body armour reduces the magnitude and changes the location of shoulder pressure and perceived discomfort in soldiers. Ergonomics. 2018;61(4):566-575. |
| Lim DS. Dermatology in the military: an East Timor study. Int J Dermatol. 2005;44(4):304-311. |
| Mahoney G, Slade GD, Kitchener S, et al. Lifetime fluoridation exposure and dental caries experience in a military population. Community Dent Oral Epidemiol. 2008;36(6):485-492. |
| Mahoney G, Slade G, Kitchener S. The true prevalence of unscheduled dental visits in the Australian Defence Force. J Mil Veterans Health. 2010;18(3):5-11. |
| McDonald D, Orr RM, Pope R. A comparison of work health and safety incidents and injuries in part-time and full-time Australian army personnel. J Athl Train. 2016;51(11):880-886. |
| McDougall L, Drummond PD. Personal resources moderate the relationship between work stress and psychological strain of submariners. Mil Psychol. 2010;22(4):385-398. |
| McGuire A, Waller M, Loos C, et al. Self-reported indicators of psychological health. Psychiatr Ann. 2009;39(2):48-55. |
| McKenzie DP, Ikin JF, McFarlane AC, et al. Psychological health of Australian veterans of the 1991 Gulf War: an assessment using the SF-12, GHQ-12 and PCL-S. Psychol Med. 2004;34(8):1419-1430. |
| McKenzie DP, McFarlane AC, Creamer M, et al. Hazardous or harmful alcohol use in Royal Australian Navy veterans of the 1991 Gulf War: identification of high risk subgroups. Addict Behav. 2006;31(9):1683-1694. |
| McKenzie DP, Creamer M, Kelsall HL, et al. Temporal relationships between Gulf War deployment and subsequent psychological disorders in Royal Australian Navy Gulf War veterans. Soc Psychiatry Psychiatr Epidemiol. 2010;45(9):843-852. |
| McKenzie DP, Sim MR, Clarke DM, et al. Developing a brief depression screen and identifying associations with comorbid physical and psychological illness in Australian Gulf War veterans. J Psychosom Res. 2015;79(6):566-573. |
| McMahon TW, Newman DG. G-Induced visual symptoms in a military helicopter pilot. Mil Med. 2016;181(11):e1696-e1699. |
| Metcalf O, O’Donnell ML, Forbes D, et al. Attention-control training as an early intervention for veterans leaving the military: a pilot randomized controlled trial. J Trauma Stress. 2022;35(4):1291-1299. |
| Metcalf O, Roebuck G, Lawrence-Wood E, et al. Gambling problems predict suicidality in recently transitioned military veterans. Aust N Z J Public Health. 2023;47(3):100038. |
| Milner A, Witt K, Maheen H, LaMontagne AD. Suicide among emergency and protective service workers: A retrospective mortality study in Australia, 2001 to 2012. Work. 2017;57(2):281-287. |
| Netto K, Hampson G, Oppermann B, et al. Management of neck pain in Royal Australian Air Force fast jet aircrew. Mil Med. 2011;176(1):106-109. |
| Newman P, Adams R, Waddington G. Two simple clinical tests for predicting onset of medial tibial stress syndrome: shin palpation test and shin oedema test. Br J Sports Med. 2012;46(12):861-864. |
| Oakes MJ, Sherman BE. Cystic hygroma in a tactical aviator: a case report. Mil Med. 2004;169(12):985-987. |
| Orme GJ, Kehoe J. Psychological adjustment and retention of Australian Army reservists following a stability operation. Mil Med. 2011;176(11):1223-1231. |
| Orme GJ, Kehoe EJ. Hardiness as a predictor of mental health and well-being of Australian army reservists on and after stability operations. Mil Med. 2014;179(4):404-412. |
| Orme GJ, Kehoe EJ. Reservists in a post-conflict zone: deployment stressors and the deployment experience. Mil Med. 2014;179(2):137-142. |
| Orr RM, Johnston V, Coyle J, et al. Reported load carriage injuries of the Australian army soldier. J Occup Rehabil. 2015;25(2):316-322. |
| Orr RM, Pope R. Gender differences in load carriage injuries of Australian army soldiers. BMC Musculoskelet Disord. 2016;17(1):488. |
| Orr RM, Coyle J, Johnston V, et al. Self-reported load carriage injuries of military soldiers. Int J Inj Contr Saf Promot. 2017;24(2):189-197. |
| Orr R, Schram B, Pope R. Sports Injuries in the Australian Regular Army. SAFETY. 2020;6(2). |
| Orr RM, Cohen BS, Allison SC, et al. Models to predict injury, physical fitness failure and attrition in recruit training: a retrospective cohort study. Mil Med Res. 2020;7(1):26. |
| O’Shea SD, Pope R, Freire K, et al. Prevalence of lower urinary tract symptoms in a cohort of Australian servicewomen and female veterans. Int Urogynecol J. 2023;34(4):885-896. |
| Pain MCF. Previous asthma and methacholine reactivity in defence force recruit screening. J Mil Veterans Health. 2005;14(1):12-14. |
| Peake J, Gargett S, Waller M, et al. The health and cost implications of high body mass index in Australian defence force personnel. BMC Public Health. 2012;12:451. |
| Pilgrim CHC, Brennan L. Surgical management of injured ADF personnel deployed to Afghanistan 2001-2021. ANZ J Surg. 2023;93(4):821-828. |
| Pope R, Orr R. Incidence rates for work health and safety incidents and injuries in Australian Army Reserve vs full time soldiers, and a comparison of reporting systems. J Mil Veterans Health. 2017;25(2):16-25. |
| Pope RP. Injury surveillance and systematic investigation identify a rubber matting hazard for anterior cruciate ligament rupture on an obstacle course. Mil Med. 2002;167(4):359-362. |
| Pope RP. Rubber matting on an obstacle course causes anterior cruciate ligament ruptures and its removal eliminates them. Mil Med. 2002;167(4):355-358. |
| Rayner SPS, Viney LL. Case study of six-year follow-up of Navy survivors of a multiple fatality fire at sea. Mil Med. 2010;175(7):514-517. |
| Rickards CA, Newman DG. G-induced visual and cognitive disturbances in a survey of 65 operational fighter pilots. Aviat Space Environ Med. 2005;76(5):496-500. |
| Roach GD, Rodgers M, Dawson D. Circadian adaptation of aircrew to transmeridian flight. Aviat Space Environ Med. 2002;73(12):1153-1160. |
| Runge CE, Waller MJ, Moss KM, et al. Military personnel ratings of a deployment and their positive and negative deployment experiences. Mil Med. 2020;185(9-10):e1615-e1623. |
| Runge CE, Moss KM, Dean JA, et al. Self-reported pain or injury from equipment used on military deployment. Occup Med (Lond). 2021;71(2):79-85. |
| Sadler N, Van Hooff M, Bryant RA, et al. A. Suicide and suicidality in contemporary serving and ex-serving Australian Defence Force personnel. Aust N Z J Psychiatry. 2021;55(5):463-475. |
| Schofield PW, Gibson R, Tavener M, et al. Neuropsychological health in F-111 aircraft maintenance workers. Neurotoxicology. 2006;27(5):852-860. |
| Schram B, Orr R, Rigby T, et al. An analysis of reported dangerous incidents, exposures, and near misses amongst army soldiers. Int J Environ Res Public Health. 2018;15(8):1605. |
| Schram B, Orr R, Pope R. A profile of knee injuries suffered by Australian army reserve soldiers. Int J Environ Res Public Health. 2019;16(1):12. |
| Schram B, Pope R, Orr R. Injuries in Australian Army full-time and part-time personnel undertaking basic training. BMC Musculoskelet Disord. 2019;20(1):6. |
| Schram B, Pope R, Norman A, et al. A detailed analysis of serious personal injuries suffered by full time and part time soldiers of the Australian Army. Mil Med. 2020;185(3-4):e364-e369. |
| Schram B, Orr R, Pope R. A profile of injuries suffered by female soldiers serving in the Australian Army. BMC Public Health. 2022;22(1):813. |
| Searle AK, Van Hooff M, Lawrence-Wood ER, et al. The impact of antecedent trauma exposure and mental health symptoms on the post-deployment mental health of Afghanistan-deployed Australian troops. J Affect Disord. 2017;220:62-71. |
| Searle AK, Van Hooff M, McFarlane AC, et al. Screening for depression and psychological distress in a currently serving military population: The diagnostic accuracy of the K10 and the PHQ9. Assessment. 2019;26(8):1411-1426. |
| Sellentin R, Jones R. The effect of core and lower limb exercises on trunk strength and lower limb stability on Australian soldiers. J Mil Veterans Health. 2012;20(4):21-35. |
| Sellentin R, Sanchez P. Review of physiotherapy records to characterise musculoskeletal injury in Australian soldiers in the 16th Air Defence Regiment. J Mil Veterans Health. 2011;19(4):7-13. |
| Selman J, Rogers R, Molloy S. Negative alcohol and tobacco consumption behaviors in an Australian army combat brigade. Mil Med. 2020;185(5-6):e686-e693. |
| Selman J, Zevenbergen M, Wing G. Estimating the proportion of overweight soldiers in the Australian Army by combat uniform waist size. BMJ Mil Health. 2022;168(5):386-390. |
| Shaw A, Newman P, Witchalls J, et al. T. Externally validated machine learning algorithm accurately predicts medial tibial stress syndrome in military trainees; a multi-cohort study. BMJ Open Sport Exerc Med. 2023;9(2):e001566. |
| Sherrard J, Lenne M, Cassell E, et al. Injury prevention during physical activity in the Australian Defence Force. J Sci Med Sport. 2004;7(1):106-117. |
| Smart TL, Singh B. Excessive daytime sleepiness in a trainee military pilot. Aviat Space Environ Med. 2006;77(7):753-757. |
| Smith A. Hypoxia symptoms reported during helicopter operations below 10,000 ft: a retrospective survey. Aviat Space Environ Med. 2005;76(8):794-8. |
| Smith C, Doma K, Heilbronn B, et al. Impact of a 5-week individualised training program on physical performance and measures associated with musculoskeletal injury risk in army personnel: a pilot study. Sports (Basel). 2023;11(1):8. |
| Steele NM, Benassi HP, Chesney CJ, et al. Evaluating the merits of using brief measures of PTSD or general mental health measures in two-stage PTSD screening. Mil Med. 2014;179(12):1497-502. |
| Steele NM, Fogarty GJ. Screening for anger and sleep difficulties. Mil Med. 2017;182(3):e1628-e1633. |
| Steele NM, Rodgers B, Fogarty GJ. The relationships of experiencing workplace bullying with mental health, affective commitment, and job satisfaction: application of the job demands control model. Int J Environ Res Public Health. 2020;17(6):2151. |
| Steele NM, Fogarty GJ, Rodgers B, et al. The effects of working in a bullying climate on psychological distress and job satisfaction: a multilevel analysis. Aust J Psychol. 2022;74(1):2125341. |
| Stewart K. Military milk: breastfeeding rates among Australian Defence Force women who return to military service following maternity leave. J Hum Lact. 2015;31(1):138-144. |
| Syed Sheriff R, Van Hooff M, Malhi G, et al. Associations of childhood trauma and childhood mental disorder with past-year mental disorder in military and civilian employed men. Psychiatry Res. 2019;280:112482. |
| Syed Sheriff R, Van Hooff M, Malhi G, et al. Associations among childhood trauma, childhood mental disorders, and past-year posttraumatic stress disorder in military and civilian men. J Trauma Stress. 2019;32(5):712-723. |
| Syed Sheriff R, Van Hooff M, Malhi G, et al. Childhood determinants of suicidality: comparing males in military and civilian employed populations. Psychol Med. 2019;49(14):2421-2431. |
| Syed Sheriff R, Van Hooff M, Malhi G, et al. Childhood trauma and the impact of deployment on the development of mental disorder in military males. Psychol Med. 2020;50(5):818-826. |
| Tait JL, Bulmer S, Drain JR, et al. Associations between inflammatory markers and well-being during 12 weeks of basic military training. Eur J Appl Physiol. 2021;121(3):849-860. |
| Tait JL, Aisbett B, Corrigan SL, et al. Recovery of cognitive performance following multi-stressor military training. Hum Factors. 2022:187208221086686. |
| Tait JL, Drain JR, Bulmer S, et al. Factors predicting training delays and attrition of recruits during basic military training. Int J Environ Res Public Health. 2022;19(12):7271 |
| Tucker B, Netto K, Hampson G, et al. Predicting neck pain in Royal Australian Air Force fighter pilots. Mil Med. 2012;177(4):444-450. |
| Van Hooff M, McFarlane AC, Davies CE, et al. The Australian Defence Force Mental Health Prevalence and Wellbeing Study: design and methods. Eur J Psychotraumatol. 2014;5:23950. |
| Varker T, Cowlishaw S, Baur J, et al. Problem anger in veterans and military personnel: Prevalence, predictors, and associated harms of suicide and violence. J Psychiatr Res. 2022;151:57-64. |
| Wade D, Mewton L, Varker T, et al. The impact of potentially traumatic events on the mental health of males who have served in the military: Findings from the Australian National Survey of Mental Health and Wellbeing. Aust N Z J Psychiatry. 2017;51(7):693-702. |
| Wallace D, Rayner S. A military second opinion mental health clinic. J Mil Veterans Health. 2015;23(3):12-17. |
| Waller M, Treloar SA, Sim MR, et al. Traumatic events, other operational stressors and physical and mental health reported by Australian Defence Force personnel following peacekeeping and war-like deployments. BMC Psychiatry. 2012;12:88. |
| Waller M, McGuire ACL, Dobson A. Alcohol use in the military: associations with health and wellbeing. Subst Abuse Treat Prev Policy. 2015;10(27):27-49. |
| Waller M, Charlson FJ, Ireland REE, et al. Time-course of PTSD symptoms in the Australian Defence Force: a retrospective cohort study. Epidemiol Psychiatr Sci. 2016;25(4):393-402. |
| Warfe PG, Jones DD, Prigg SK. Developing injury prevention strategies for the Australian Defence Force (Reprinted from Aust Mil Med. 2000;9:3-8). J Mil Veterans Health. 2011;19(3):45-49. |
| Warner R, Avery JC, Neuhaus S & Davies MJ. Australian Veterans of the Middle East conflicts 2001–2010: select reproductive health outcomes. Part 1 — maternal and paternal outcomes. Fertility & Reproduction. 2020; 2(2):43-52. |
| Warner R, Avery JC, Neuhaus S & Davies MJ. Australian Veterans of the Middle East conflicts 2001–2010: select reproductive health outcomes. Part 2 — prenatal, fetal, and neonatal outcomes. Fertility & Reproduction. 2020;2(2):53-60. |
| Warner R, Avery JC, Neuhaus SJ, Davies MJ. Associations between environmental exposures in the Middle East Area of Operations and pregnancy outcomes in Australian Defence Force veterans. Environ Res. 2022;208:112688. |
| Watterson J, Gabbe B, Dietze P, et al. Piloting an injury awareness and education program for reducing alcohol-related harm in navy trainees. J Subst Use. 2018;23(1):74-78. |
| Watterson JR, Gabbe B, Dietze P, et al. A randomized controlled trial of the Prevent Alcohol and Risk-related Trauma in Youth program in reducing alcohol-related harms in young naval trainees. Mil Med. 2023. 188(5-6):e1125-e1131. |
| Weinrauch P, Sharwood P. Employment in the Australian Army after Anterior Cruciate Ligament Reconstruction – A Pilot Study of 3 Year Postoperative Outcomes. J Mil Veterans Health. 2006;15(1):15-17. |
| Williams O, Ross VR, Lau CL, et al. Epidemiology of cruciate ligament reconstruction in the Australian Defence Force and predictors of outcome. BMJ Military Health EPub ahead of print. 2022;0:0-6. |
| Wright B, Forbes A, Kelsall H, et al. ‘Post-deployment appraisal’ and the relationship with stress and psychological health in Australian veterans. Soc Psychiatry Psychiatr Epidemiol. 2015;50(12):1885-1892. |
| Wright BK, McFarlane AC, Clarke DM, et al. Symptom attribution and symptom reporting in Australian Gulf War veterans. J Psychosom Res. 2015;79(6):674-9. |
| Wright BK, Kelsall HL, Sim MR, et al. Quality of life in Gulf War veterans: the influence of recency and persistence of psychiatric morbidity. Appl Res Qual Life. 2019:14:23–38. |
| Wright BK, Kelsall HL, Clarke DM, et al. Symptom attribution and treatment seeking in Australian veterans. J Health Psychol. 2020;25(10-11):1498-1510. |
| Zheng WY, Kanesarajah J, Waller M, et al. Childhood adversity and traumatic exposures during deployment as predictors of mental health in Australian military veterans. Aust N Z J Public Health. 2016;40(1):10-15. |
Reasons for exclusion of studies included: non-primary data study (n=91), non-health outcome (n=57), former serving ADF members (n=21), data not presented separately for current serving ADF members (n=11), non-ADF military personnel (n=9), malaria outcome (n=4), and systematic review that only analysed studies that were already included in the search (n=2).
In addition to the studies identified through database searching, a further 60 reports and theses were included in the catalogue. The Department of Defence provided 33 reports, and one of the authors (HK) sourced 24 reports and three PhD theses through a grey literature search.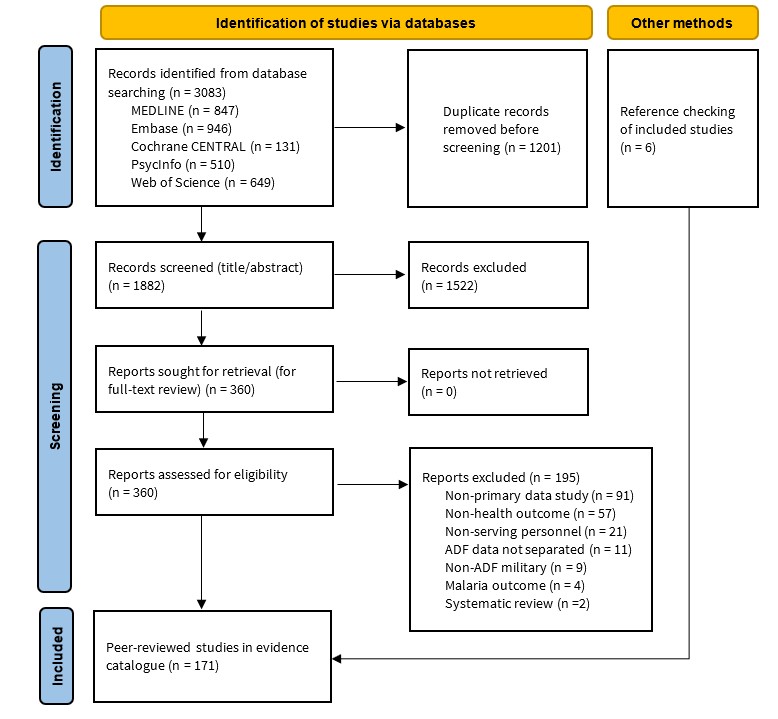
Figure 1. Preferred Reporting Items for Systematic Reviews and Meta-Analysis–Scoping Reviews (PRISMA–ScR), flow chart of the scoping review, 1 January 2002 to 24 April 2023.
Study characteristics
The 171 studies used the following study designs: cohort (n=71), analytical cross-sectional (n=45), prevalence (n=17), RCTs (n=14), quasi-experimental (n=9), case reports (n=4), diagnostic test accuracy (n=4), systematic review (n=3), case control (n=3), and qualitative (n=1). There were studies published in every year between 2002 and 2023, with a large number published in 2017–2023 (Table 1).
Table 1: Peer-reviewed publications investigating the health of ADF members 2002–2023 by publication time period and top three priority health research areas n (% of total for time period)
| Year of publication | Total no. of studies | No. of mental health and wellbeing studies | No. musculoskeletal studies | No. occupational and environmental studies |
| 2002–2006 | 33 (19) | 11 (33) | 8 (24) | 8 (24) |
| 2007–2011 | 27 (16) | 8 (30) | 5 (19) | 8 (30) |
| 2012–2016 | 39 (23) | 19 (49) | 11 (28) | 2 (5) |
| 2017–2021 | 49 (29) | 27 (55) | 15 (31) | 5 (10) |
| 2022–2023 | 23 (13) | 13 (57) | 7 (30) | 0 (0) |
| TOTAL | 171 | 78 (47) | 46 (27) | 23 (13) |
Note: Studies may be assigned to multiple categories (maximum of three) so percentages will not sum to 100.
All studies were Australian-based, although there was collaboration with authors from the United States of America (USA), the United Kingdom (UK), Canada, the Netherlands and Belgium. Two of the systematic reviews reported data from the USA, UK and an unspecified international source. A large proportion (n=83, 48%) of studies received funding from the Department of Defence or Department of Veterans’ Affairs. The remainder of studies were funded by charitable organisations (n=21), research councils/government scheme (n=6), internal funding (n=16), other (US Army, Australasian Military Medicine Association) (n=2), and 44 studies did not state their funding source; some of those studies analysed data sets collected by the Department of Defence (n=7).
The 60 research reports and theses spanned the years 2003–2023, with the majority (77%) published in the most recent decade, 2012–2023 (Table 2). Australian authors and research teams authored all reports and theses.
Table 2: Reports and theses publications investigating the health of ADF members 2002–2023 by publication time period and top three priority health research areas (PHRA) n (% of total for time period)
| Year of publication | Total studies in top 3 PHRA for time period | Mental health and wellbeing | Musculoskeletal | Occupational and environmental |
| 2002–2006 | 5 (8) | 2 (40) | 1 (20) | 3 (60) |
| 2007–2011 | 9 (15) | 8 (89) | 0 (0) | 7 (78) |
| 2012–2016 | 13 (22) | 10 (77) | 3 (23) | 11 (85) |
| 2017–2021 | 26 (43) | 18 (69) | 1 (4) | 7 (27) |
| 2022–2023 | 7 (12) | 6 (71) | 0 (0) | 1 (14) |
| TOTAL | 60 | 44 (72) | 5 (8) | 29 (48) |
Note: Studies may be assigned to multiple categories (maximum of three) so percentages will not sum to 100.
Risk of bias assessment
Sixteen of the included studies were assessed as having a high risk of bias; these were cohort, analytical cross-sectional, case-control and systematic review studies. The critical domain in the cohort, analytical cross-sectional and case-control studies was confounding factors: studies that did not consider possible confounding factors within the analysis were considered to have a high risk of bias. In addition, one cohort study was assessed as high risk of bias due to a considerable non-random loss to follow up. The systematic review was rated as high risk of bias due to insufficient methodological detail. All of the RCTs, quasi-experimental studies, prevalence studies, qualitative studies, diagnostic test accuracy studies and case report studies were either moderate or low risk of bias. Analytical cross-sectional studies had the highest proportion of high-risk-of-bias assessments (Table 3).
Table 3: Risk-of-bias assessment for study types in catalogue of ADF studies 2002–2023 n (%)
| Type of study | Low risk of bias | Moderate risk of bias | High risk of bias | TOTAL (n=171) |
| Cohort | 32 (45) | 33 (46) | 6 (9) | 71 |
| Cross-sectional analytical | 26 (58) | 11 (24) | 8 (18) | 45 |
| Case report | 4 (100) | – | – | 4 |
| Case control | – | 2 (67) | 1 (33) | 3 |
| Prevalence | 13 (76) | 4 (24) | – | 17 |
| Quasi-experimental | 4 (44) | 5 (56) | – | 9 |
| Qualitative | – | 1 (100) | – | 1 |
| Diagnostic test accuracy | 2 (50) | 2 (50) | – | 4 |
| Systematic review | 1 (33) | 1 (33) | 1 (33) | 3 |
| Randomised control trial | 8 (57) | 6 (43) | – | 14 |
Evidence catalogue development
It proved challenging to attribute any identified research studies to two of the strategic priority areas: ‘health of the future war fighter’ (focus on the health needs of Defence members in the future, exploring technological advances, emerging technologies and innovative models of care) and ‘health system performance and efficiency’. No published studies were identified that could be catalogued under these priority areas.
There were considerably more studies involving mental health and wellbeing outcomes than any other priority area (Table 4). Most mental health and wellbeing studies (76%) were published in the last decade. Thirty-one studies contained health outcomes that could not be categorised into the predefined eight priority health areas and were categorised under ‘other health outcomes’. This category included the following health outcomes: dental (n=7); neurological (n=7); respiratory (n=4); auditory (n=4); melanoma (n=1); other dermatological conditions (n=1); and general health (n=7). In total, 16 of these studies involved only one health outcome outside the strategic priority health areas (seven dental studies, three neurological studies, six general health studies). The remaining 15 studies also included one of the predefined health area outcomes and were therefore catalogued in both.
Table 4: Studies investigating the health of ADF members 2002–2023 by priority health research area
| Health domain outcome |
Number of peer-reviewed publications (n=171) |
Reports/ theses (n=60) |
TOTAL (n=231) (%) |
| 1. Measuring and monitoring the health of the force | 16 (9) | – | 16 (7) |
| 2. Health of the future warfighter | 0 (0) | 0 | 0 |
| 3. Musculoskeletal injuries | 46 (27) | 5 (8) | 51 (22) |
| 4. Occupational and environmental health | 23 (13) | 29 (48) | 52 (23) |
| 5. Mental health and wellbeing | 78 (45) | 44 (73) | 122 (53) |
| 6. Health system performance and efficiency | 0 (0) | 0 | 0 |
| 7. Gender and health | 23 (13) | – | 23 (10) |
| 8. Infectious diseases | 2 (1) | – | 2 (1) |
| 9. Other health outcomes | 31 (18) | – | 31 (13) |
Note: Studies may be assigned to multiple (maximum of three) categories; therefore, percentage and count will exceed 100.
The majority of studies focused on mental health and wellbeing (n=78, 47%), followed by musculoskeletal disorders (n=46, 27%) and occupational and environmental exposures (n=23, 13%). No studies on traumatic brain injury-related research were identified. When examining the 126 studies funded by the Department of Defence and the Department of Veterans’ Affairs, the distribution across priority health research areas was similar to the overall totals.
Consistent with the published literature, the reports and theses also showed that the majority (72%) focused on mental health and wellbeing outcomes (Table 2). Occupational and environmental health-related outcomes were included in approximately 48% of reports and theses, and musculoskeletal outcomes were included in 8%.
Discussion
This scoping review resulted in the development of an extensive evidence catalogue of health research involving ADF members over 20 years. One hundred and seventy-one peer-reviewed journal articles and 60 reports/theses were identified, appraised and catalogued according to the ADF health research priorities.
Most health research involving ADF members over the previous 20 years has focused on mental health and wellbeing (53%), with the next most common health area being musculoskeletal injuries (22%). Over the period 2002–2011, there was a more even distribution of studies across domains, including: mental health and wellbeing (32%); musculoskeletal disorders (22%); and occupational and environmental health (27%). However, over the period 2012–2022, there was an increased emphasis on mental health and wellbeing research (53%) and a decrease in research investigating musculoskeletal (30%) or occupational and environmental health (6%) outcomes. This may reflect recent greater recognition of the impact of military service on mental health and wellbeing outcomes, not only by Defence and the Department of Veterans’ Affairs, but also by researchers and the wider community. Notably, women have been eligible to serve in non-combat roles in the ADF since the 1970s, but have only been eligible to apply for all roles since 2014. There were more studies from 2014 onwards investigating gender and health outcomes; of the 23 studies included in this category, only five were published before 2014.
There has been a sustained focus on research into musculoskeletal injuries and disorders among ADF members throughout the past 20 years. This would seem appropriate, since musculoskeletal disorders are the second most common reason for workers’ compensation claims within the ADF.10 Similarly, musculoskeletal injuries and disorders also make up the majority of compensation claims within the Australian civilian workforce.11 However, notably, of the 46 musculoskeletal disorder studies, 19 related to musculoskeletal disorders that developed during periods of mandatory basic training. There are practical benefits to undertaking research during basic training, and it is desirable to identify strategies to prevent these injuries, which might detriment recruitment. However, the relative lack of studies among current serving ADF members beyond basic training may be an important gap to address, as the majority of musculoskeletal injuries resulting in workers’ compensation claims are likely to occur post-training.
Evidence has demonstrated that poor mental health and wellbeing can be associated with musculoskeletal injuries and disorders and chronic pain.12-14 However, very few studies (n=3) of ADF members took a holistic approach to exploring the incidence of musculoskeletal disorders; almost half of the studies focused on physical health outcomes in basic military training15-17 without collecting concurrent outcomes on mental health and wellbeing. It seems that this is consistent with contemporaneous studies involving overseas military forces, such as the US military, which have also considered only physical factors in the aetiology and prevention of musculoskeletal injuries, rather than adopting a biopsychosocial approach to health.18-21 There are additional challenges in the military workforce due to the nature of the work and working conditions with unpredictable and often changeable environments in which they operate. This may at least partly explain the small number of studies that investigated prevention strategies. The limited investigation into the prevention of musculoskeletal disorders and injuries across the life span indicates a future priority area for health research.22
Most studies included in the evidence catalogue were based on research commissioned and/or funded by the Department of Defence or the Department of Veterans’ Affairs. Studies that were not funded by the Department of Defence or the Department of Veterans’ Affairs had Department of Defence Veterans’ Affairs HREC approval to include ADF personnel participants. No matter who commissioned the studies, the outcomes focused predominately on mental health and wellbeing.
While mental health and wellbeing-related studies were particularly prevalent, mental health conditions only accounted for a relatively small number of compensation claims in 2021/2022,10 and an even smaller proportion of work, health and safety incidents (1% in 2012/2014 in the Army).15 The highest number of claims for military compensation relate to hearing loss,10 yet only four studies considered this health outcome.23-26 The search strategy did not actively exclude trauma or traumatic brain injury. However, no articles relating to research on trauma or traumatic brain injury research and current serving ADF personnel were retrieved. Several studies have reported the prevalence of post-traumatic stress disorder (PTSD) in cohorts of current serving ADF members, with findings ranging from 2% to 11% prevalence,27-32 but there was heterogeneity in the diagnostic criteria utilised. A 2010 report about the mental health of ADF personnel found the 12-month prevalence of mental health disorders (22%, 95%CI 18.9–25.3%) was similar to that of the general Australian population (20.7%, 95%CI 18.9–25.3%), but that lifetime prevalence rates were higher in ADF members (54.1% vs 49.3%).29 Furthermore, the estimated prevalence for affective disorder in ADF members was higher over both the previous 12 months (9.5% vs 5.9%) and lifetime (20.8% vs 14.0%), compared to the general Australian population.33 Suicide rates within current serving ADF members are lower than the general Australian population and stable over the last 20 years. However, suicide rates for former serving ADF members were estimated to be 26% higher among men and 107% higher among women compared to the general population.34 The relatively low previous 12-month prevalence of mental health disorders and overall suicide rate among current serving ADF members may be at least partly attributed to the ‘healthy-worker effect’.35
Overall, a substantial body of research investigating health outcomes has been undertaken among ADF members over the past 20 years. The research has informed an evidence base for health policy and practice, in Australia and overseas, and has developed military and veteran health research capability within Australia. It is anticipated that the new ADF Health Strategy4 and an evidence catalogue will inform an approach to a) address knowledge gaps in health research relating to strategic priority areas; b) target future health research to areas that will help improve capability and economic benefits for the ADF; and, c) improve health outcomes for ADF personnel, their families and the Defence community.
This study has several strengths. It was a comprehensive, systematic search of the published literature across the five relevant electronic databases and handsearching, with a focus on a well-defined population. The search followed rigorous methodology consistent with best-practice standards, and bias risk was assessed using valid tools. Unfortunately, due to the heterogeneity of study designs and outcome measures, it was not possible to undertake any meta-analysis. Studies that examined the health outcomes of former serving ADF members and the consideration of the translation of research findings into policy and practice were outside the scope of this review. However, an evidence catalogue for ex-serving members could be beneficial.
Conclusion
An evidence synthesis catalogue of health research involving ADF members over the past 20 years has been developed. Since 2002, there has been a considerable number of research studies investigating the health of ADF members, the majority of which focused on mental health and wellbeing or musculoskeletal outcomes. Cataloguing past health research has provided insights into the importance of aligning research focus with ADF priorities. It provides an opportunity to consider strategies to ensure that future health research aligns closely with ADF priorities.
Declarations
Any views expressed in this review are those of the authors, not the Department of Defence.
Ethics approval
Not applicable
Consent for publication
All co-authors have reviewed the final version of the manuscript and expressed their consent for publication.
Availability of data
All data generated or analysed during this study are included in this published article.
Competing interests
The Department of Defence employs ZJ, EW and JS. No other competing interests are declared.
Funding
The Commonwealth of Australia (represented by the Defence Science and Technology Group) supported this research through a Defence Science Partnerships agreement (Ref: ID11922).
Corresponding Author: Helen Kelsall, helen.kelsall@monash.edu
Authors: N Kinsman1, H Kelsall1, D Tomic1, S Green2, A Collie3, S McDonald2, Z Jenkins4, E Wessel4, J Saboisky4, K Walker-Bone1
Author Affiliations
1 Monash University – Monash Centre for Occupational and Environmental Health, School of Public Health and Preventive Medicine
2 Monash University – Cochrane Australia, School of Public Health and Preventive Medicine
3 Monash University – Healthy Working Lives Research Group, School of Public Health and Preventive Medicine
4 Australia Department of Defence


